AAMC Recommendations for COVID-19 Testing: The Current State and The Way Forward
Testing for COVID-19 must increase rapidly and dramatically
The novel coronavirus, or SARS-CoV-2, and the disease it causes, COVID-19, present the world with a particularly insidious problem. The deadly virus, which has already killed more than 220,000 Americans and 1 million people worldwide, spreads rapidly and efficiently from person to person. Approximately 40% of those infected have no symptoms but are still contagious,1 and therefore we cannot rely on reported symptoms or hospitalization rates alone to locate, isolate, and suppress the virus. At the same time, we know that most Americans are still vulnerable to the virus, with less than 10% carrying the antibodies that may indicate immunity.2 We need a science-driven approach to track and suppress the virus, and one major component of this strategy must be increasing the available and effective COVID-19 diagnostic, screening, and surveillance tests. (See AAMC’s Guide to Tests and Testing for a discussion of COVID-19 test types and uses.) Moving beyond this pandemic will require strategic and robust testing in coordination with well-established public health measures to eradicate the disease.
Opening schools, universities, businesses, and public gathering spaces with safety and confidence requires a new commitment to developing and manufacturing tests and a strategic and coordinated use of available tests. The AAMC recommends that a national pandemic response should seek sustained and regular testing targets for effective diagnosis and screening. At the virus’s current prevalence and infection rate, at a time when new cases are increasing daily, the United States should be able to administer over 800,000 diagnostic tests and over 8 million screening tests to test as many as 9 million people each day.
Improvements in testing technology and availability have increased daily test rates to near 1 million per day, but we are far short of the number of tests which should be administered daily under current conditions. A commitment to increasing the number of tests and suppressing the virus requires dedicated funding; continued investment in technology and test development; and smarter, more strategic use of our resources.
-
How many — and what kind of — tests should the United States be doing?
-
We need transparent and coordinated action to increase testing
View related resources for more information about testing.
How many — and what kind of — tests should the United States be doing?
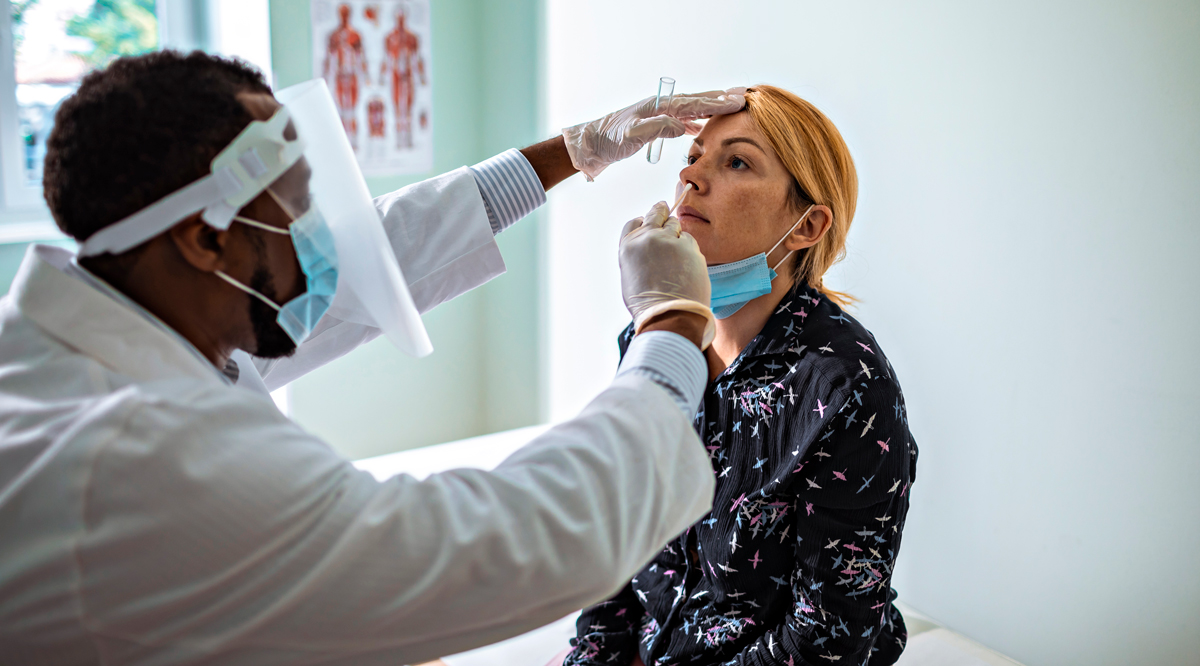
The AAMC noted in July 2020, as daily cases were falling, that the United States would need to test at least 2.3 million people per day to decrease the rate of positive tests below 3%.3 Our failure to contain the spread of the virus in the first several months of the pandemic has resulted in a much higher number of tests needed now. The AAMC’s assertion that a pandemic response currently requires 9 million people per day to be tested represents an estimation of the need for immediate testing in the categories below. See Appendix A for the assumptions and estimations used to develop minimum testing strategies.
Up to 800,000 diagnostic tests are needed for:
- Each person who is symptomatic.
- Close contacts of every positive case identified (whether symptomatic or asymptomatic).
Over 8 million screening tests are needed for:
- Every person who enters a health care facility for an inpatient admission or outpatient surgery.
- Routine testing of all health care providers in hospital settings.
- Routine testing of first responders (law enforcement officers, paramedics, and EMTs).
- Strategic sampling of residents in nursing homes and assisted living facilities.
- Strategic sampling of incarcerated individuals.
- Strategic sampling of residents and staff in homeless shelters.
- Routine testing of every K-12 teacher.
- Strategic sampling of K-12 students.
- Strategic sampling of college and university students, faculty, and staff.
This is not an exhaustive list of the categories of individuals that should be routinely tested. Additional testing is needed for other essential workers and individuals such as contact tracers, delivery and retail personnel, employees of agricultural and meatpacking businesses, and public transportation employees.
What would change the needed number of tests?
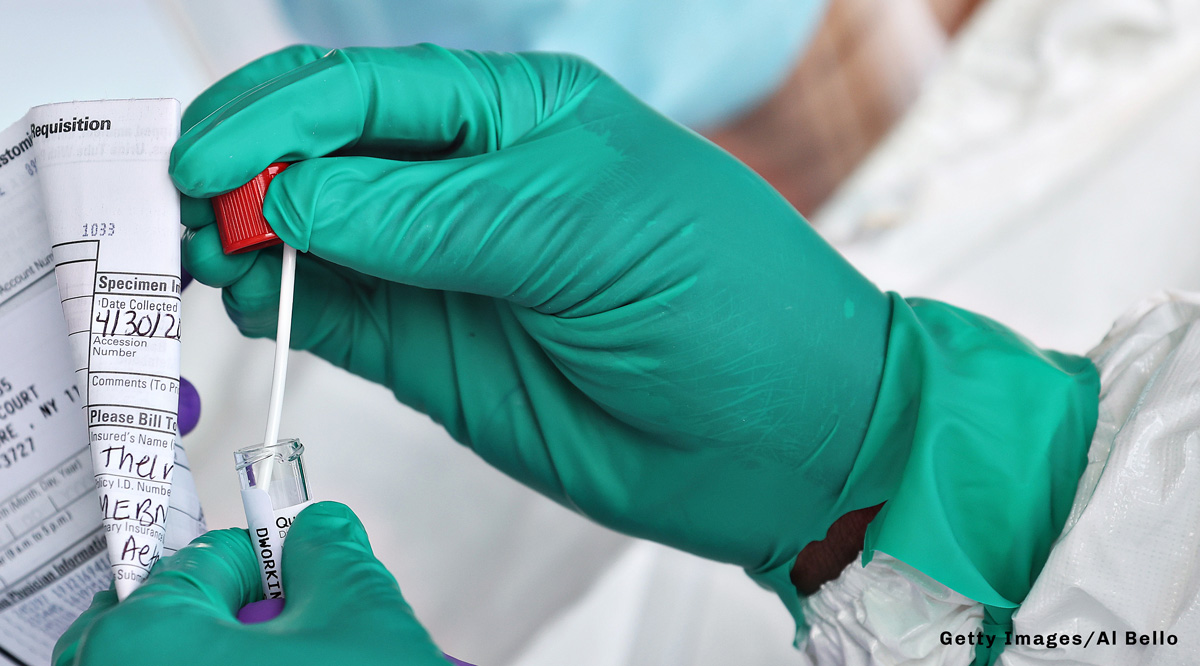
The testing targets described above reflect the current COVID-19 status of the United States. Surges in infection rates (or failure to follow recommended public health measures for controlling the virus) could require increases in diagnostic or screening testing needs. High vaccination levels will likely decrease or alter testing needs.
Surveillance measures such as testing of wastewater, surfaces, and air quality must continue and provide powerful indicators of the presence and spread of the virus but are not included in the testing targets. As better surveillance testing increases the ability to quickly detect the virus’s presence or absence in a community or population, the need for individual screening tests could decrease if the virus is not detected.
Vaccines, when administered to a large percent of the population, can confer immunity to those in the population who are vaccinated. As the percentage of those vaccinated increases, the number of diagnostic and screening tests needed will decrease. However, the need for antibody tests will increase. Antibody tests that detect neutralizing antibodies in the blood of people who have been vaccinated will help public health departments understand the level of immunity in communities. “Herd immunity” describes a circumstance in which enough people in a population are immune to the virus that the virus no longer spreads through the community as a whole. Herd immunity for COVID-19 can only be achieved through vaccination, not by letting people become infected with SARS-CoV-2. Attempting to address the pandemic through greater infection will cost countless lives unnecessarily.
Why aren’t there enough tests now?

As of mid-October, the United States had conducted approximately 110 million tests4 since the beginning of the pandemic. That means that in more than seven months, we have only done approximately half of the number of tests we should be doing each month to control and respond to the spread of the virus. While recent advances in testing technologies are improving testing capability, that increase is too slow to meet current needs. According to the COVID Tracking Project, the seven-day rolling average of tests performed during the month of July gradually increased from 650,000 to 825,000 tests per day but remained under 800,000 per day for the next six weeks. This is less than 10% of what the AAMC estimates daily testing targets should be at this time.
Several organizations have proposed various testing models that conclude that between 1 million and 14 million people should be tested each day, depending on the testing goal being advanced by each report and when in the pandemic the testing model was released. (See Appendix B for a discussion of existing proposals from other organizations.) All agree that the United States is nowhere near where it needs to be to move forward as a nation with confidence on the state of COVID-19.5 Even current estimates of available tests from manufacturers or the federal government are only a fraction of the number of tests that are needed under current conditions. We do not have the tests that we need due to three primary causes: manufacturing and supply chain concerns that have hampered the ability to scale up testing capacity, uncontrolled spread of the virus, and variable state policies and strategies.
-
Manufacturing and supply chain failures plagued the initial rollout of diagnostic tests and continue to date.6 Routine backlogs and shipment delays of test kits, reagents, PCR machines, swabs, or transport media still prevent clinical labs from being able to match the demand for symptomatic individuals and patients receiving care in hospitals. The months long inability to meet diagnostic testing needs overshadowed the additional needed focus on expanding screening capacity. As a result, laboratories doing RT-PCR diagnostic tests are competing for scarce resources with the labs using the same types of machines and reagents for RT-PCR screening tests.
-
Poorly contained spread of COVID-19 has greatly increased testing needs. As initial hot spots began to show a decrease in new cases and hospitalizations, other areas of the country began to show dramatic increases in infection. A sudden spike in cases per day that began in late June following inconsistent state reopening plans quickly drove the nation’s diagnostic testing needs far beyond what was previously needed. Future planning must accommodate the potential for spikes in multiple areas of the country.
-
A federal response that resulted in variable state policies and testing strategies has made it difficult to assess testing needs, compare state approaches, or ensure consistent strategies. Instead of a uniform federal approach to testing that set specific targets based on population, risk, and COVID-19 prevalence, states were asked to come up with their own testing strategies. In many cases, positivity rates fluctuated as daily tests decreased and increased over time.
We need transparent and coordinated action to increase testing

To refine a comprehensive strategy and move toward achieving the necessary volume of tests, we need the following:
- A clear and transparent national testing strategy.
- A coordinated focus on current testing targets to keep schools, businesses, and public gathering places open with confidence.
- A functional partnership between the federal government, state health authorities, academic institutions, and industry to fund and accelerate screening and surveillance testing.
A national testing strategy
As the impact of COVID-19 continues to disrupt and devastate communities, health care systems, the economy, schools, and businesses — with a disproportionate impact on communities of color — the need for a comprehensive national testing strategy has never been so urgent. The calls for such a strategy have echoed for months,7 and recent calls to action underscore that the importance of a national strategy has only increased. Recent revisions in basic guidelines from federal agencies about who should be tested and how the virus is spread from person to person communicate a lack of clarity and have moved us further from a true comprehensive, science-driven plan. A national strategy must issue granular standards and directives with an expectation that each state will implement the strategy according to the same standards and criteria.
We have an opportunity to better understand and respond to the disparate impact of COVID-19 on vulnerable and underserved communities with a coordinated effort to collect essential race and ethnicity data in concert with expanded routine testing. The addition of testing and infection rate data would allow a better response to the pandemic, when it is combined with “information on the social and environmental conditions in which people live, work, and play (e.g. crowding, access to food, housing security, etc.) that impact how illness can spread.”8
As part of this strategy, the AAMC renews its call to make all federal efforts to increase testing capacity fully transparent. Testing supplies should not be scarce this many months into the pandemic, yet clinical and academic labs facing rising demand in the face of increasing routine reports that ordered testing supplies are canceled (or delayed with the explanation that they have been redirected by the federal government) — without any insight into how or where those supplies are being used. A truly coordinated effort to address this problem as a nation should involve cross-sector decision-making followed by publicly available information about what quantities and types of testing supplies are being redirected.
With a national strategy and specific targets and benchmarks for success, the federal government would be in a better position to marshal the resources and expertise at its disposal to address supply chain, manufacturing, and access to testing issues. The Defense Production Act (DPA) can be a powerful tool in focusing the nation’s resources but needs to be part of a coordinated and transparent strategy. Each use of the DPA for testing supplies, from swabs to reagents to rapid antigen tests, should be listed on a publicly available website with information about the supply type being manufactured, the amount of the supplies that will be made available, and the timeline and details for distribution of those supplies.
Testing is occurring in commercial labs, point of care settings, clinical labs, academic labs, and research labs, and it may expand to at-home settings. As part of a deliberative national strategy, we must not continue the current approach that has labs competing with each other for the same testing supplies from the same sources. New avenues of testing must ensure that current supply chains are not further disrupted but are developing parallel testing processes and supplies.
A coordinated focus on a single testing goal
There is no question that increasing testing remains a powerful tool against the spread and recurrence of COVID-19. Even after one or more vaccines are available for use, it may be many months or years before a safe, effective, and readily accessible vaccine is both widely available and widely used. The need to have reliable testing for the virus will thus remain an essential component of the United States’ ability to identify and control the virus. The number of tests needed depends on the specific end being targeted and the strategic deployment of those tests to reach that end.
Any testing approach must make a clear distinction between the number of tests needed to determine whether a specific person has COVID-19 for purposes of making further recommendations about that person’s health (diagnostic testing) and the number of tests needed to not only test asymptomatic individuals suspected of being exposed but also to test large numbers of people on a routine basis through screening and surveillance testing. As vaccination increases, those tests may shift to antibody testing to measure population-level immunity levels.
Strategic use of testing technologies means using the most appropriate tests for each purpose. In general, the more important it is to get accurate results for a single test, the more sensitive a test should be. Such tests are often, but not always, more costly and resource-intensive to run. The use of highly sensitive tests for surveillance purposes or less accurate tests for diagnostic or critical screening purposes could be misdirecting resources and could have negative impacts on individual or public health.
A multi-stakeholder partnership to move forward
Advances in innovation and new testing technologies are accelerating the speed at which new tests are becoming available. Incentive mechanisms like the National Institutes of Health (NIH) Rapid Acceleration of Diagnostics (RADx) program seek to fund promising new surveillance testing technologies.9 Simpler testing processes with fewer steps and thus fewer needed supplies are working to mend broken links in the supply chain. Yet we remain in a siloed environment where tests are developed and conducted in “micro-communities” — with access to tests and the likelihood that a test will be recommended for an individual being determined by geographic location, institutional affiliation, test funder, or reimbursement practices.
Only in a functional partnership with federal leadership across stakeholder groups can we achieve an adequate testing capacity in a manner that is rapid, scalable, and equitable. This collaboration must include as equal partners federal and state agencies, test developers, CLIA-certified commercial and clinical labs, research labs, and large institutions conducting broad surveillance testing. A collective and transparent approach to increasing testing capacity can achieve greater efficiency and capacity. At the same time, such collaboration can serve to increase and maintain public trust in the development, deployment, and reporting of tests for COVID-19.
The testing recommendations and call to action issued by the AAMC Research and Action Institute today were authored by Heather Pierce, JD, MPH, AAMC senior director for science policy and regulatory counsel, and Ross McKinney, Jr., MD, AAMC chief scientific officer. We are appreciative of the review and input from the following experts as these recommendations were being developed:
Richard J. Bookman, Ph.D., Director, UHealth Care Lab, University of Miami Miller School of Medicine
Priscilla Markwood, CAE, Executive Director, Association of Pathology Chairs (APC)
Megan L. Ranney, MD, MPH, Associate Professor of Emergency Medicine, Assistant Dean of Brown Institute for Translational Sciences, Director of the Brown-Lifespan Center for Digital Health, Associate Professor of Health Services, Policy and Practice
1 Estimated by the CDC, July 2020.
2 Anand S, Montez-Rath M, Han J, et al. Prevalence of SARS-CoV-2 antibodies in a large nationwide sample of patients on dialysis in the USA: a cross-sectional study. Lancet. September 25, 2020. doi: 10.1016/S0140-6736(20)32009-2.
3 Association of American Medical Colleges. The Way Forward on COVID-19: A Road Map to Reset the Nation’s Approach to the Pandemic. https://www.aamc.org/covidroadmap/roadmap. Accessed October 15, 2020.
4 Estimated by the COVID Tracking Project by aggregating state reports.
5 A Government Accountability Office September 2020 report, COVID-19: Federal Efforts Could Be Strengthened by Timely and Concerted Actions, concurred with this assessment (https://www.gao.gov/assets/710/709492.pdf).
6 American Society for Microbiology. Supply shortages impacting COVID-19 and non-COVID testing. https://asm.org/Articles/2020/September/Clinical-Microbiology-Supply-Shortage-Collecti-1. Published October 15, 2020. Accessed October 15, 2020.
7 Association of American Medical Colleges. Letter to Dr. Birx. https://www.aamc.org/media/44011/download. Published April 13, 2020. Accessed October 15, 2020.
8 Association of American Medical Colleges. AAMC calls for enhanced COVID-19 data collection on health disparities. https://www.aamc.org/news-insights/press-releases/aamc-calls-enhanced-covid-19-data-collection-health-disparities Published April 10, 2020. Accessed October 15, 2020.
9 Association of American Medical Colleges. Re: request for information- inviting comments and suggestions on university-based approaches for COVID-19 surveillance testing to review the current landscape. https://www.aamc.org/media/47786/download. Published August 26, 2020. Accessed October 15, 2020.