It may be less inspiring than gene splicing, robotic surgery, or an artificial pancreas, but the growing wave of mergers, acquisitions, and partnerships is a formidable force in medicine today. In fact, says Janis M. Orlowski, MD, AAMC chief health care officer, the phenomenon is “dramatically changing the face of academic medicine.”
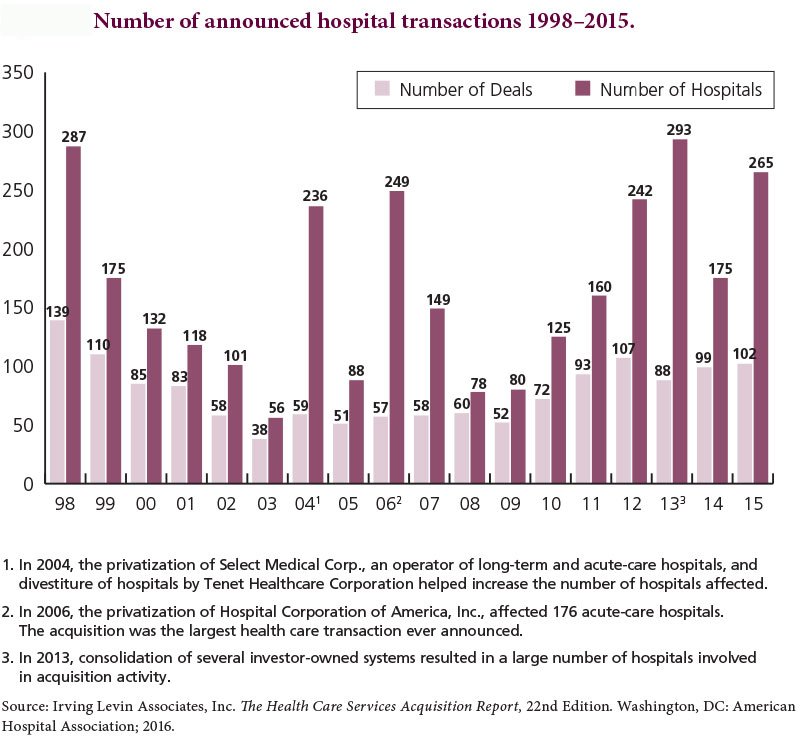
The numbers support this claim: Between 2003 and 2015, U.S. hospital mergers and acquisitions more than doubled, according to the American Hospital Association, and in a recent survey, three-quarters of hospital leaders indicated that they were involved in or contemplating some type of merger, acquisition, or partnership.
To educate academic medical leaders about this growing trend and its implications for medical schools, teaching hospitals, and health systems, the AAMC Advisory Panel on Health Care conducted an 18-month study of this issue. The new AAMC report, Hospital Mergers, Acquisitions, and Partnership Strategies: Implications for Academic Medicine, explores the factors driving mergers, acquisitions, and partnerships (MAP) activity, as well as the effects of consolidation. It also offers guidance on all stages of the process, from dipping an exploratory toe into MAP waters to achieving success after taking the plunge.
The report notes that there are many possible financial benefits of MAP—increased access to capital and more leverage with insurers, among others—as well as various pluses for research and care derived from larger population and referral pools.
At the University of Colorado Denver, for example, a joint venture has allowed academic and community hospitals to share data, expertise, and important quality and safety measures. “It has pulled everybody up,” says Lilly Marks, vice president for health affairs of the University of Colorado and Anschutz Medical Campus and AAMC Board member.
But, the report cautions, consolidation efforts sometimes can erode an institution’s priorities and resources. Consider this case: One institution spent more than $30 million and 18 months on a merger attempt that never materialized. And completed MAP activities also can have risks. These include winding up with a disappointing partner as well as unanticipated threats to an institution’s assets, stability, and reputation in the community.
Mergers and medical schools
In the current environment, schools of medicine may face greater risks from MAP activity than teaching hospitals do, the report notes. Much of the threat lies in a tough reality: Medical schools are increasingly dependent on financial support from affiliated clinical enterprises.
In addition, post-MAP, medical school teaching faculty and researchers can feel underappreciated, overly corporatized, and cut out of governance structures, Orlowski says. Staff at teaching hospitals also may face similar issues after combining with a nonteaching hospital.
“My advice is ... don’t think you’ll work out issues when the time comes. Deal with the hard problems up front.”
Lilly Marks, University of Colorado Denver
To help avoid such divides, academic leaders at the University of Colorado Denver School of Medicine arranged with their clinical affiliate, UCHealth, to present information at each board meeting on the value of teaching and research. A speaker would, for example, explain how a certain area of biomedical research contributes to patient outcomes.
Without such efforts, misunderstandings can flourish, Orlowski has found. “We heard [from a clinical entity’s leaders], ‘We’re giving them so much money, $80 million, to support research and education,’” she recalls. “Then we went across to the [academic] office, and we heard, ‘They’re so stingy, they’re giving us a measly $80 million.’ The two sides had a common understanding of the dollar amount,” she notes, “but not of the purpose and value that the investment brought.”
Making MAP work
In identifying key steps that can help ensure success, MAP veterans stress good communication. Employees need to understand why the activity is happening, how it benefits both parties, and what will unfold, experts advise. At the time of its merger, for example, Yale New Haven Health System even set up a 24/7 command center to address any employee concerns.
Also crucial to success is the blending of cultures. Different communications styles, different decision-making structures, and for-profit versus nonprofit status all can hobble institutions’ integration.
Failing to understand existing culture can even impact the bottom line, notes R. Kevin Grigsby, AAMC senior director of member of Member Organizational Development. At one institution with a culture of distrust, for example, faculty members spent an inordinate amount of time serving on committees in an effort to protect their own interests. AAMC's Engagement Solutions, which helps organizations address issues that impact their performance, identified ways to increase trust, which cut down on wasted faculty effort and, ultimately, saved the organization nearly $1 million.
To help successfully blend the cultures of merging institutions, experts recommend thoughtful planning. “Some groups have actually developed a strategic plan using cultural assessment tools to help the development of a new culture,” says Orlowski. “Initially, I thought, ‘That’s strange. You can’t force culture.’ But as I read about some of the plans, I saw that in order to have a new and positive culture, it must be fostered.” Culture-related plans address everything from employees’ titles to how to conduct meetings of the merged groups.
Colorado's Marks advises advance decision making in other areas as well, such as how faculty physicians and community physicians interrelate to a newly merged institution. "You have to think very carefully about how you create the structure of this organization," she says. "My advice is, and I can't emphasize this strongly enough, don't think you'll work out issues when the time comes. Deal with the hard problems up front."
Paul Klotman, MD, president, CEO, and executive dean of Baylor College of Medicine, has overseen both successful and failed MAP activities. He highlights the need to create systems for collaboration. After Baylor formed a joint venture with the much larger Catholic Health Initiatives (CHI), he detected a major issue: Few people understood the agreement. "Four people of the 50,000 employees at CHI understood the agreement, and three on our side [did]," explains Klotman. The result was several roadblocks, such as CHI staff rejecting Baylor requests for information. So the institutions established a joint management team to meet regularly and review topics of mutual concern.
Issues remain, Klotman adds, but on the whole the venture has achieved many goals, including preserving numerous jobs. “It’s been extremely good for us. Every time I sit here and feel it’s been difficult ... I always think about where we are relative to where we would be had we not done it,” he says. “We just have to continue to work at making it better.”
