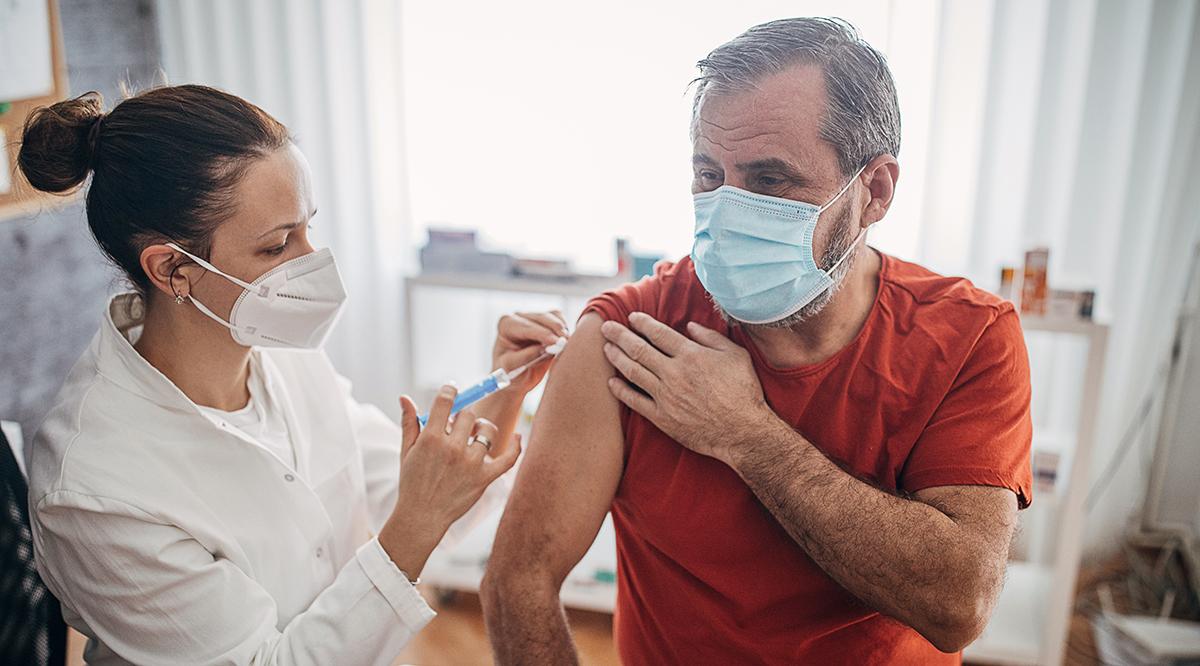
Like many in their small, rural town of Front Royal, Virginia, Everett and Kristin Jiles — who describe themselves as Christian conservatives — were on the fence about getting a COVID-19 vaccine.
Eventually, afraid that her underlying asthma could lead to complications if she got sick, Kristin, 56, got her first shot in April 2021. But Everett, 59, stood firm.
“You had all these different views being pushed and no idea who to believe,” he says. “It just felt wrong, so I was against it.”
Everett’s attitude toward vaccination changed in July, however, when the couple had contact with a relative carrying the delta variant. Both contracted COVID-19. That gave them a chance to conduct their own informal study comparing the course of the disease with and without the protection of a vaccine.
At first, their symptoms seemed to track in the same direction, but after a week of severe headache, fatigue, and sinus symptoms, Kristin recovered while Everett’s health declined. A few days later, he was admitted to the intensive care unit with a high fever and pneumonia in both lungs. He would be in the hospital for 15 terrifying days.
As Everett lay in his hospital bed struggling to breathe, “I asked Kristin to take my picture and put it on Facebook and tell people, ‘You don’t want to end up like this,’” he says. “‘Just get the shot, because if I had just gotten the shot, none of that would have happened.’”
Now the couple are crusaders for COVID-19 vaccines, urging everyone they know to roll up their sleeves. They don’t want others in their or any other conservative, rural community to have to face a life-threatening coronavirus infection or see a loved one die to change their minds about vaccines.
Our experience “was proof for us that the vaccine worked,” Kristin says.
Yet, the task they and public health experts face is formidable. Many people in rural and conservative areas remain frustratingly resistant to vaccination, challenging public health officials to come up with more convincing — and sensitive — approaches to promoting greater vaccine uptake.
When attitudes don’t budge
A preprint study from the University of Pittsburgh Graduate School of Public Health, using county and state data collected in the months since the vaccines became available early this year, underscores this resistance.
While overall vaccine confidence rates have increased nationally, “the same percentage of people who were strongly against getting the vaccines in January were still strongly against [getting them] in May,” says study author Wendy C. King, PhD, an associate professor of epidemiology at the school.
In fact, after accounting for other factors that can skew the results like age, sex, race, employment status, and education, “people in very rural counties are 23% more likely to be vaccine hesitant than someone living in a city,” she says.
The data also showed that people in counties with the highest support for former President Donald Trump in the 2020 presidential election were 44% more likely to be vaccine hesitant, King says. Those living in a state with a Republican governor were 34% more likely to be hesitant than people living in a state with a Democratic governor.
“One of the biggest issues that we are facing as a country is that masking and vaccination have become partisan,” says Rachael Lee, MD, associate professor of infectious diseases at the University of Alabama at Birmingham Health System.
But politics alone don’t explain the disparate statistics. Debate over the virus and the vaccines have exposed cultural fault lines that date back generations, according to Edwin Leap, MD, an emergency medicine doctor who grew up in West Virginia and now serves rural hospitals in North and South Carolina.
“People in rural America are a culture. They tend to be fiercely independent,” he says. “The very last way you’ll get them to comply is by telling them they better do what’s right. They’re not going to have you tell them what to do.”
Decades of economic decline have also stoked resentment between town and country and helped fuel distrust of public institutions and government.
What can be done about lagging vaccination rates in America’s rural pockets? Health and communications experts have some ideas.
Just provide the facts.
Like Leap, Julia Daisy Fraustino, PhD, co-founder of the Public Interest Communication Research Lab in the West Virginia University Media Innovation Center, says a heavy-handed approach to promoting vaccines — such as using appeals that could be perceived as decrees or commands — is bound to fail among conservative, rural populations. The lab has studied barriers to vaccination in the overwhelmingly rural state, which may resonate in similar areas around the country.
“Frankly, in West Virginia, we’re scrappy, we’re resilient, and we love our freedom and independence,” she says. “People want to make their own decision about vaccinations. Just giving them unbiased basic information to make an informed decision is the best way to move forward with this.”
Leave politics at the door.
“The politicization of COVID-19 in this group is incredibly influential and it turns them off very severely,” Fraustino says. “So avoiding anything even remotely political with this group is important.”
She concedes that it can be tricky. “Things that one person would never even remotely consider political [are] perceived as absolutely political to another person,” she says. So, tread carefully.
If it comes up, Lee responds this way: “This virus does not care who you are, what you believe.” That takes the discussion out of the political sphere. “Then you can address the patient’s concerns,” she says.
Ally with community “influencers.”
Rural populations consider their local health care professionals the most trusted source of COVID-19 vaccine information, says Lisa Costello, MD, MPH, assistant professor of general pediatrics at West Virginia University School of Medicine. “Fact-based vaccine recommendations from a community doctor, nurse, pharmacist, or community health worker are taken incredibly seriously,” she says.
“The family medicine doctor who is embedded in a rural community is going to have much more sway than someone like me — an infectious disease doctor who may not have a relationship with the patient,” Lee agrees. “That’s what really will drive change.”
Though it’s lagging behind other states now, West Virginia’s vaccine rollout initially led the states, likely because it relied on a network of small, locally owned pharmacies and community pharmacists to get shots in arms, Fraustino explains.
Don’t refute false claims about the vaccines.
“We tend to want to address things that we perceive as misinformation, but in doing so, it’s very common for us to repeat those rumors or misinformation,” she says. “People can forget whether you agreed or disagreed with it, but you actually reinforce it accidentally in the person’s mind in the process of refuting it.”
Fraustino suggests providing positive vaccine information without repeating the falsehood. For instance, if someone says that vaccines give you COVID-19, you don’t have to say they don’t give you COVID-19. Instead, provide an answer that addresses the vaccine’s overall safety — why and how they’re safe.
Treat people with care and respect.
Regardless of a patient’s worry or belief, it’s important to take their concerns seriously and treat them respectfully. Appeals based on guilt or shame aren’t just unprofessional, they’re also ineffective.
“People won’t be persuaded by people who look at them with disdain,” Leap says.
Fraustino agrees. “If people perceive that they’re being judged or shamed in any way, that turns them off — it can actually boomerang in the opposite direction, whereas they might otherwise have been open to vaccination,” she says.
Similarly, “people want to be talked with, not down to, and that's all in how a message is conveyed,” says Amy Elizondo, MPH, chief strategy officer at the National Rural Health Association in Washington, D.C. “It's about hearing somebody’s concerns and talking them through that.”
A conversation with her doctor affirmed Angela Fain’s decision to receive the shot. Sensitive to what she perceived as pressure to get vaccinated, Fain, 57, of Leavenworth, Kansas, whose husband serves in the military, took issue with blanket vaccine recommendations.
“The publicity is, ‘Let’s protect everybody else,’” says Fain, who has a history of unusual allergies. “How about we protect the individual and worry about what’s best for them?”
When she finally went to get her first dose in September, she says, “I told the doctor I had been on steroids because of summer allergies, and she was like, ‘Oh, you need to come back in two weeks [to allow time for the steroids to leave her system].’ So I was very comforted and that made me trust the system more. She really was looking out for my particular health, not somebody else’s.”
Be prepared to play the long game.
It’s probably going to take more than one conversation to really change someone’s intentions, Costello says. When you’re wrapping up with an unvaccinated patient, give them a call to action, such as offering additional resources to learn about the efficacy of the vaccine and inviting them to come back and talk about it more so that you can answer any other questions.
“This is a personal decision for folks,” Elizondo explains. “Those one-on-one conversations are where the most impact is had, and where outcomes are more positive.”
Although having multiple conversations might be frustrating and time-consuming, the strategy pays off.
“If people take the time and effort to engage in those long-term conversations — fact-based, judgment-free, shame-free — over and over again and really listen,” says Fraustino, “perceptions do shift.”
This article first appeared on VaccineVoices.org.