Few American families are untouched by heart disease. Heart-related illnesses are responsible for 1 in every 4 deaths in the United States and for millions of dollars in health care expenses annually.
America’s medical schools and teaching hospitals have pioneered many of the most effective innovations in cardiac care. Academic medicine continues to push the frontiers of knowledge and treatment forward through research and the training of next-generation caregivers and innovators.
Advances in heart disease diagnosis in adults
Today, adults who suffer from heart-related illnesses benefit from advances in the prevention, diagnosis, and treatment of heart disease developed in the nation’s teaching hospitals and halls of academic medicine. Those advances have led to significantly better survival rates and improved quality of life.
In the United States, more than 28 million people — 1 in 10 adults — have been diagnosed with heart disease. Coronary heart disease (CHD) is the most common form of heart disease, resulting in over 700,000 people suffering heart attacks each year and over 370,000 deaths. But between 2004 and 2014, the death rate attributed to CHD fell 35.5% and the number of related deaths declined 19.2%.
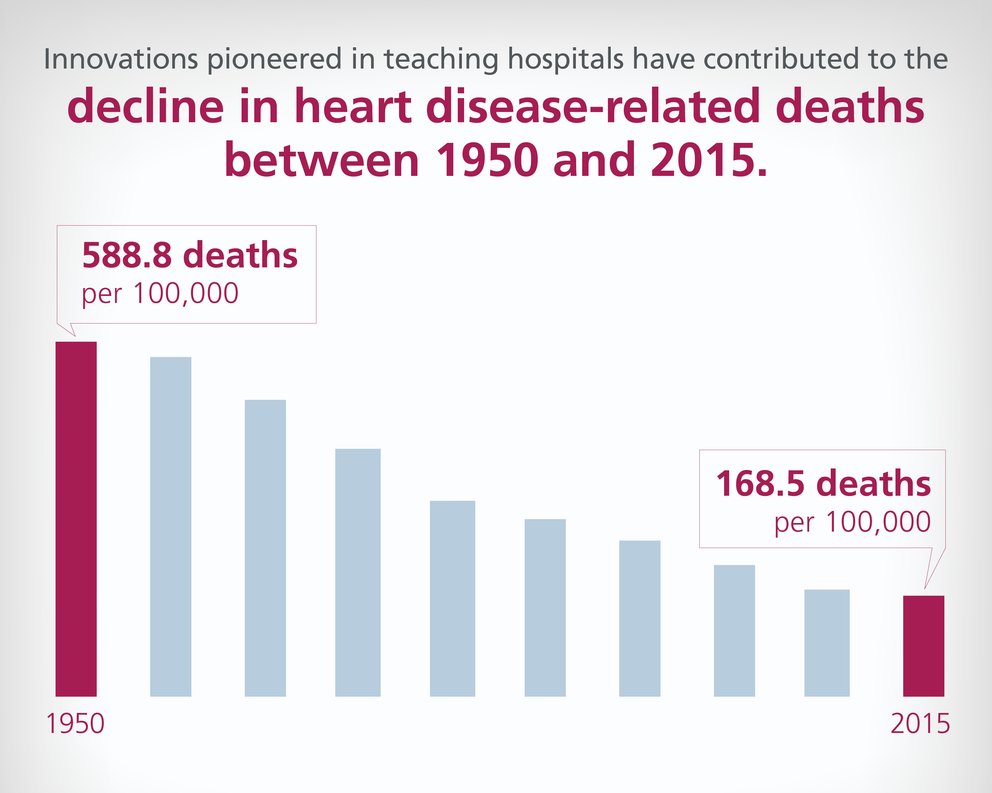 National Center for Health Statistics, Health, United States, 2016 — Individual Charts and Tables: Spreadsheet, PDF, and PowerPoint files. https://www.cdc.gov/nchs/data/hus/2016/017.pdf
National Center for Health Statistics, Health, United States, 2016 — Individual Charts and Tables: Spreadsheet, PDF, and PowerPoint files. https://www.cdc.gov/nchs/data/hus/2016/017.pdf
Experts estimate that advances in disease prevention — including aggressive efforts to reduce the underlying causes of heart disease such as hypertension, diabetes, smoking, and high cholesterol — account for approximately 44% of the reduction in mortality.
Academic medicine supports CAD prevention and early diagnosis
Academic medicine ensures that emerging medical practitioners are equipped to provide evidence-based care for coronary artery disease (CAD). The academic medicine community has made significant contributions not only to the identification of risk factors but to successful approaches to the diagnosis and management of these risks.
Teaching hospitals in particular played a key role in demonstrating that treating patients diagnosed with moderate hypertension reduced cardiac-related deaths. They were also at the forefront of identifying and understanding other risk factors, such as hypercholesterolemia, or high cholesterol. That groundbreaking work led to three U.S. medical school faculty members winning Nobel Prizes in 1964 and 1985 for their work on cholesterol and cardiovascular disease.
Academic medicine continued to collect data and share study results with community-based physicians and physician trainees to establish a new standard of care called primary prevention, which has become an effective approach to reducing CAD illness and death.
Teaching hospitals develop new CAD interventions
Today, life-saving cardiac surgery and other diagnostic and therapeutic procedures stand on deep foundations laid by academic medicine’s pioneering work. Innovative approaches to diagnosing internal blockages in coronary arteries paved the way for effective surgical and other therapeutic interventions.
For example, physicians at the Cleveland Clinic (OH) and the University of Oregon, now Oregon Health & Science University (OHSU), pioneered the use of coronary angiography to diagnose CAD. These diagnostic breakthroughs built on the earlier work of two medical professors from Columbia University who won a Nobel Prize, along with a German physician, “for their discoveries concerning heart catheterization and pathological changes in the circulatory system.”
Teaching hospitals also pioneered new therapeutic interventions such as open-heart coronary artery bypass graft (CABG) procedures. These treatments would not have been possible if physicians at Stanford Medical Center (CA), Sidney Kimmel Medical College at Thomas Jefferon University (PA), and& Mayo Clinic (MN) had not developed heart-lung machines, solved perfusion issues, and trailblazed new surgical techniques.
Teaching hospitals also advanced less invasive catheter-based approaches, which open coronary artery blockages with balloons or stents in a procedure known as percutaneous transluminal cardiac angioplasty.
Even though teaching hospitals treat some of the sickest and most medically complex patients, they outperform nonteaching hospitals in 30-day survival rates for both CABG and heart attack admissions. Some of the reasons for these outcomes include:
- Faster cardiac event intervention. Cardiologists say “time is muscle” because the more quickly a heart attack can be treated, the better the patient’s chances are for survival. Since teaching hospitals support 24/7 access to specially trained physicians who are available to perform diagnostic and therapeutic procedures, they may have improved patient outcomes.
- More surgical experience. Experts suggest that patient outcomes may be related to the number of cases performed by the operating team. Teaching hospitals tend to perform high volumes of cardiac surgery and interventional cardiology procedures.
- Greater ability to address complications. Patients at teaching hospitals have the advantage of 24/7 access to sophisticated equipment, specialized physicians, and cardiac ICU staffs. As a result, if complications arise, critical resources are more likely to be available.
Pioneering heart valve disease intervention
Heart valves can malfunction due to age and other degenerative causes, congenital defects, or illnesses such as rheumatic fever, side effects of radiation therapy, and when heart valves do not work properly, complications such as heart failure and stroke may result.
In the mid-20th century, the first artificial heart valves were developed, and academic physicians at Georgetown University School of Medicine (DC), OSHU School of Medicine (OR), Harvard Medical School (MA), and many other teaching institutions have continued to improve them. These innovations offer real hope to valve disease patients.
Today, ongoing advancements — many of which have been developed, tested, evaluated, and/or refined at America’s medical schools and teaching hospitals — allow patients requiring cardiac valve replacement the ability to choose less risky, less invasive, and less costly treatment alternatives.
For example, physicians now can replace valves without traditional open-chest approaches, using minimally invasive ports. In procedures pioneered at academic medical centers such as Stanford Medical Center and the Cleveland Clinic, surgical robots and even nonsurgical catheter-based approaches are options.
Adult heart transplants and ventricular assist devices
Even with the advances in prevention of and care for cardiac disease, some hearts are beyond mending. But with the innovations pioneered in academic medicine, critically ill patients are offered increased hope through heart transplantation surgery and ventricular assist devices.
With the first human-to-human heart transplant performed 50 years ago at Baylor College of Medicine (TX) — and building on early attempts at Maimonides Medical Center and Stanford Medical Center — the procedure is giving a new chance at life to patients with hearts damaged beyond repair. In 2017, more than 2,800 adults received heart transplants in the United States, which is an 80% increase from just over 1,500 in 1988 and 22 in 1975.
Early transplant results were far from optimal due to problems of host-donor incompatibility and rejection. Academic medicine, however, continued to advance knowledge in the areas of tissue typing and immunosuppression which, along with advances in surgical techniques, have contributed to vastly improved outcomes for heart transplant patients. As of 2015, one-year, three-year, and five-year adult primary heart transplant survival rates exceeded 90%, 84%, and 78%, respectively. In fact, perhaps the greatest problems facing potential adult heart transplant patients today is the shortage of organs available for transplant, with more than 3,800 adults on heart transplant waiting lists as of April 2018.
For some patients on the donor list for heart transplants, their survival is maintained through ventricular assist devices (VAD), an electromechanical device for assisting cardiac circulation, which is used either to partially or to completely replace the function of a failing heart. For patients with heart failure who are unable or unlikely to receive a transplant, long-term use of VADs may be appropriate.
Since first being implanted in a patient by Baylor College of Medicine faculty member Michael DeBakey, MD, in 1969, VADs have undergone numerous improvements designed to make them smaller, lighter, more reliable, fully implantable (without any connection to an external device), and less prone to complications. Many of these life-saving innovations, including several currently underway, have emerged from America’s medical schools and teaching hospitals.
Innovation continues generation to generation
Through research and evaluation, academic medicine continues to push the boundaries by improving the prevention and treatment of adult cardiac disease.
Academic medicine is responsible for assuring that medical students, residents, and fellows go into their communities prepared to bring state-of-the-art, evidence-based medicine to their patients and to continue academic medicine’s traditions of continuous discovery and improvement.
In addition, improvements in cardiac care outcomes reflect the development of very specific diagnostic and therapeutic techniques in cardiology and cardiac surgery. Better outcomes for cardiac patients reflect broader efforts, often developed and championed by medical schools and teaching hospitals, to improve the quality, safety, and value of health care provided to all patients.
