5 Stories of Survival, Made Possible by Academic Medicine
These stories have been repurposed with permission from: University of Iowa Health Care Patient Stories, UC Davis Health Patient Stories, Texas Children’s Hospital Patient Stories, University of Florida Health Stories, and OU Health Blog.
When families are facing their darkest moments, academic medical centers offer something few other institutions can: hope, backed by cutting-edge science. These five stories — and countless others like them — highlight how expertise, empathy, and integrated teams make the impossible possible. They are powerful reminders of why academic medicine matters for patients, for families, and for the future of health care.
Nash, the world’s most premature baby
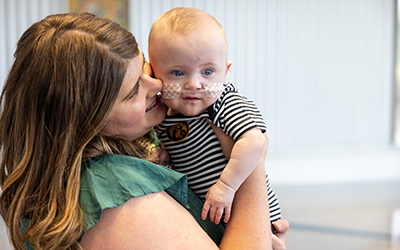
Photo credit: University of Iowa Health Care Patient Stories
When Nash Keen was born, he weighed just 10 ounces, less than a can of soda. His journey is one of medical innovation, relentless teamwork, and the unique capabilities of University of Iowa Health Care’s Stead Family Children’s Hospital, one of the few places in the world equipped to treat babies born so early.
Nash’s birth came just after crossing the hospital’s 21-week threshold for active intervention — timing that high-risk obstetrician Malinda Schaefer, MD, PhD, called “a new frontier in maternal-fetal medicine.” A multidisciplinary team of 21 neonatologists, nine NICU fellows, and dedicated nurse practitioners, nurses, respiratory therapists, dietitians, pharmacists, physical and occupational therapists, and more sprang into action. They inserted a breathing tube — an extraordinary feat for a baby so small — and began targeted organ support using hemodynamic monitoring, a technique pioneered at University of Iowa that allows clinicians to modify treatment based on real-time assessments of heart function and blood flow.
“When he was first born, his blood pressure was really low,” said neonatologist Amy Stanford, MD. “With hemodynamics, we could see that his heart was functioning well, so we adjusted our approach.” This precision medicine approach cuts the chance of death or major brain bleeding in very premature babies in half.
Over the next six months in the NICU, Nash underwent surgery, received dozens of medications, and was monitored around the clock. “They were on top of it every step of the way,” said his father, Randall Keen. “They made sure we were well-informed and kept us involved in all the decision-making.”
Today, Nash is learning, playing, and growing like any other two-year-old. His Guinness World Record-breaking outcome reflects the strength of academic medicine: a blend of cutting-edge science, collaborative care, and compassion that gives even the smallest, most vulnerable patients a chance at life.
“Every patient teaches us something,” said Stanford. “And we use those lessons to improve care for the next.”
Christina, a breast cancer survivor turned advocate

Photo credit: UC Davis Health Patient Stories
As a senior engineer with California’s Department of Water Resources, Christina Kashiwada has spent her career managing high-stakes projects — including during the 2017 Oroville Dam emergency, where her team averted a disaster that could have flooded communities for miles. She’s also a mother of two, a marathon runner, and a Spartan Race competitor.
But when she noticed a small bump on her chest — something she first brushed off as a pimple — she faced a new type of high-stakes situation. A family member urged her to call UC Davis Health, and within 48 hours, Kashiwada had undergone a mammogram, an ultrasound, and a biopsy. At just 36 years old, she was diagnosed with breast cancer.
What followed was more than a treatment plan; it was an entire academic medical center mobilizing around her. Her oncologist, Candice Sauder, MD, ensured Kashiwada never felt like just another patient. “To this day, when I see Dr. Sauder in the hallway she’ll say, ‘How’re your parents?’ She remembers us all,” Kashiwada said.
That personal care extended to Kashiwada’s entire support system. Her father attended every appointment, carrying a binder with every detail. Her mother paused her own career to care for Kashiwada and her children through chemotherapy. And the team at UC Davis Health worked together seamlessly for five years, supporting Kashiwada as she underwent surgeries, reconstruction, radiation, chemotherapy, and countless appointments.
In 2024, Kashiwada marked five years in remission. She’s back to work, back to running, and back to the family life she loves — but with a new perspective. “I’m a new person. I started a new life. I got back in it, but this was my wake-up call,” she said. Now, Kashiwada uses her experience to help others. “I am trying to be an advocate for everybody I know about preventative medicine and how you can help your body be healthy,” she said.
Kashiwada’s new outlook on life shows the power of whole-person care meeting world-class science. Her best advice? “Find a health care team that you trust.”
Bayliss, a 10-year-old rare cancer survivor
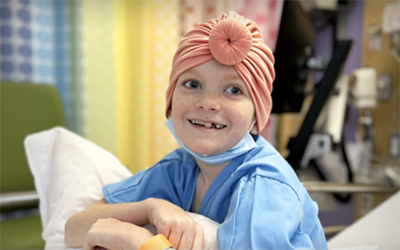
Photo credit: Texas Children’s Hospital Patient Stories
When Bayliss Filtsch, a spirited 10-year-old girl from San Antonio, complained of a stomachache, her mom didn’t expect anything out of the norm. But soon, their world was turned upside down: Bayliss was diagnosed with Stage 4 liver cancer — an aggressive form that had already spread to both of her lungs.
This cancer is so rare that fewer than 100 children are diagnosed with it each year in the United States. After initial treatments in San Antonio, Bayliss’ family turned to Texas Children’s Hospital in Houston — one of the only academic medical centers in the country with a dedicated Liver Tumor Program and a multidisciplinary team experienced in treating rare pediatric cancers.
From their first conversation, Bayliss’ care team gave her family something they desperately needed: hope. A network of pediatric experts — including oncologists, surgeons, pathologists, and interventional radiologists — worked together to create a tailored treatment plan. When conventional therapies stopped working, the team proposed trying a newer drug, pembrolizumab, which had shown promise in adults but was unproven in children.
“She was really frail. Within a week of starting it, she began improving on all fronts,” said Andras Heczey, MD, director of the Liver Tumor Program. “I will always remember calling her mom for a quick check-in a few days after starting the treatment and her saying that Bayliss felt better than she had in months.”
Today, Bayliss is cancer-free and back at school, doing the things she loves — painting, playing with friends, going to school, and just being a kid. Her story is a testament to the role of academic medical centers, which offer not only the best in patient care, but access to pioneering treatments like pembrolizumab.
“It was truly a miracle,” said Annie Filtsch, Bayliss’ mom.
Alecia, making medical history

Photo credit: University of Florida Health Stories
Ten years ago, Alecia Cosey lost consciousness behind the wheel on the way to church and awoke to her daughter’s panicked voice: “Momma, are you okay? Did your heart stop?” This was one of many emergencies Cosey had faced since she was diagnosed at just 25 years old with dilated cardiomyopathy, a genetic condition that had claimed her father’s life at 36.
“I honestly thought, ‘I only have 10 years of life left.’ Who was going to take care of my daughter?” she said.
Cosey sought treatment at University of Florida Health’s Congenital Heart Center with cardiologist Mustafa Ahmed, MD. As her condition worsened, her care team recommended a biventricular assist device (biVAD) — an implantable, mechanical pump that supports both sides of a failing heart. It’s a rare device and one that requires a team of surgical, cardiac, and transplant experts to manage. At first, Cosey was hesitant. “I prayed to the Lord. I said, ‘I need the A-Team for this surgery.’ And lo and behold, I got the A-Team,” she said. The A-Team at UF Health performed the biVAD implantation in 2019.
The device kept her alive for over three years. Cosey called herself a “bag lady,” as she carried two battery packs with her everywhere — her lifeline while awaiting a transplant. Then in 2022, a sepsis infection required emergency surgery to remove the defibrillator. Her A-Team knew the risk was grave and, once again, performed a delicate and successful surgery to remove the infected device. With the sepsis gone and 30 pounds lost, Cosey had finally cleared the last hurdle to be listed for transplant.
Then came the life-changing call: “We have a heart for you.”
The transplant was a success. Just 12 hours after, a physical therapist came to Cosey’s room, ready to get her moving. It was the moment she had dreamed about for years — free of battery packs and fear, her new heart beating strong inside her chest. Later, Cosey would learn that she had made medical history: after 1,212 days, she had become the longest-living patient in the country to successfully bridge from a biVAD to a heart transplant.
Today, Cosey is not only surviving, she’s thriving as a mother and grandmother and no longer fears not having enough time with her family. After enduring so much uncertainty, UF Health restored her hope.
“Now that she has had this incredible journey,” said Ahmed, “her body has finally caught up to that incredible spirit of hers.”
Harry, a veteran with a second chance

Photo credit: Harry Blanton
Harry Blanton, a Navy veteran from Ardmore, Oklahoma, knew something was wrong when suddenly, a severe headache and dizziness left him struggling to walk straight. Within 24 hours, he was in the ICU — his heart racing, blood pressure soaring, and blood sugar climbing to life-threatening levels, despite never having diabetes.
The diagnosis: a rare adrenal tumor, pheochromocytoma, that was flooding his body with adrenaline and pushing his vital signs to the brink. Blanton’s doctor gave him a dire warning: “If you do not have that mass removed now, you will die.”
He was referred to the University of Oklahoma (OU) Health, where he met Sanjay Patel, MD, a urologic oncologist with extensive experience treating rare tumors. “We’ve taken care of so many of these cases that we know the drill,” said Patel, who has removed nearly 50 pheochromocytomas — an exceptionally high number for such a rare condition. This expertise, along with Patel’s compassion and calm demeanor, was an immediate comfort for Blanton and his family.
“He sat down and drew pictures of my entire system inside my body,” Blanton said. “He used this analogy about group projects in school; how there’s always one person who wants to do a lot more and be in charge, and one who doesn’t want to do much. That’s what was happening with my adrenal glands.”
Blanton would need surgery to remove the tumor, but not before his case was reviewed by a team of coordinated specialists — including a cardiologist who discovered a heart abnormality. This information was essential for the care team as they prepared for the operation.
“We were texting each other, calling each other,” Patel said. “It’s impressive how everyone steps up.” This close communication extended to Blanton, too. Even on weekends, Patel personally called Blanton to check in — small gestures that made a big difference. Though Blanton’s tumor was one of the largest Patel had seen at nearly 10 centimeters, the OU Health team successfully removed it using a minimally invasive robotic surgery — a safer, more precise option than traditional open surgery.
Today, Blanton is back at home, enjoying retirement and spending time with his grandchildren. His journey from an emergency room, to treatment at OU Health, to no longer needing to take insulin, demonstrates the value of academic medical centers, which care for patients with some of the most rare and complex cases.
“We’re not just individual doctors working independently,” said Patel. “We’re an integrated system where specialists work together, communicate constantly, and bring their collective expertise to bear on saving lives.”