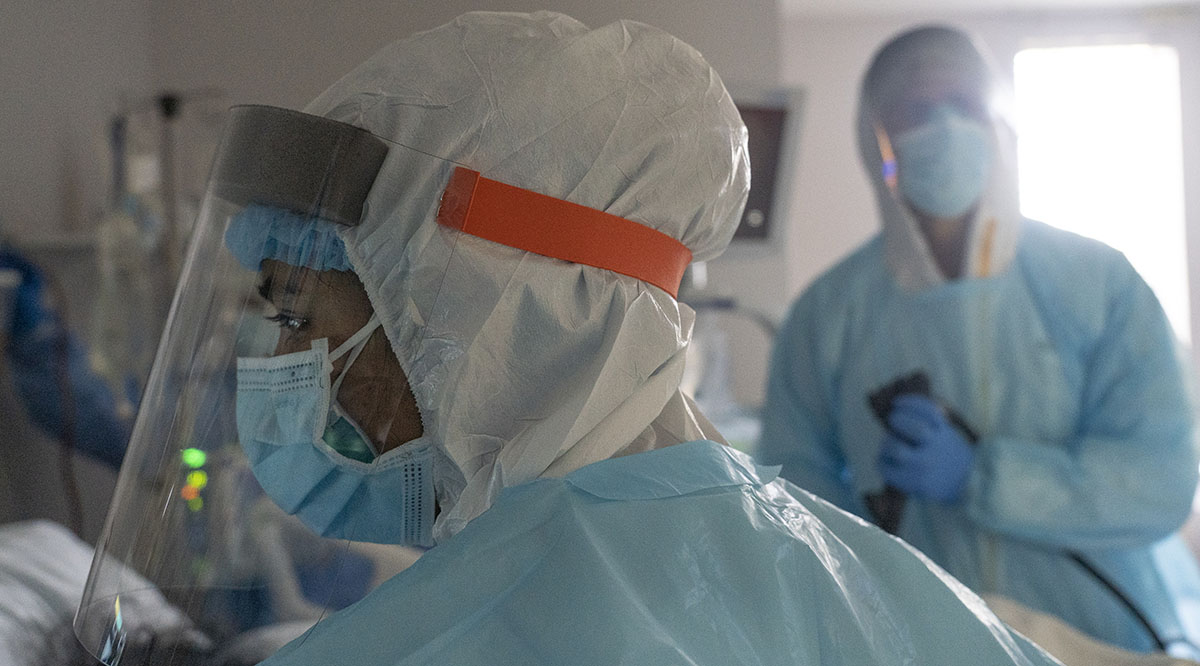
Physicians who work with emergency and critical care patients are no strangers to stressful and heartbreaking shifts, even on holidays.
But for many of those who worked in hospitals this Thanksgiving, the day was particularly intense.
As COVID-19 cases, hospitalizations, and deaths climbed in the days before the holiday, some doctors in hot spots faced full hospitals, strained staff, and the emotional toll of bearing bad news to patients and loved ones. Across the country, front-line doctors were anxious about what they fear will be an even darker and more difficult couple of months ahead, even as they felt grateful for their hardworking colleagues and hopeful about the promise of an imminent vaccine.
Physicians from several academic medical centers shared their stories with AAMCNews about what it was like to spend Thanksgiving on the front lines of the pandemic.
Laura Selby, DO, infectious diseases fellow at the University of Nebraska Medical Center (UNMC) in Omaha

It’s always hard for Selby when one of her patients dies, but it is particularly distressing when it happens on a holiday. She lost two patients this Thanksgiving weekend, one of them to COVID-19.
“You want there to be happy families and people getting better around the holidays,” Selby says. “It hits just a little bit harder.”
COVID-19 cases climbed in Nebraska through the first part of November and the UNMC, like so many hospitals in hard-hit states, had been filling up for weeks.
“It’s a daily struggle with making sure we have enough beds,” she says. “We’re all pretty tired and emotionally drained right now.”
In spite of the heaviness surrounding the pandemic, Selby found some bright spots from her holiday shift. The hospital staff was more festive than usual, and many patients were particularly grateful to the health care workers. One patient thanked her for working on the holiday and she was so touched that she almost burst into tears.
After her shift, she warmed up a frozen Thanksgiving dinner from Trader Joe’s and called her family in Oregon on Zoom. She hasn’t been able to visit home in six months but is nevertheless grateful that she lives alone during this time, so she doesn't bring the virus home to loved ones.
Larissa Velez, MD, professor and vice chair of education in emergency medicine at UT Southwestern Medical Center in Dallas

On the Thursday, Friday, and Sunday of Thanksgiving weekend, Velez worked the 7 a.m. to 4 p.m. shift. Her husband, also an emergency room doctor, worked the 3 p.m. to midnight shift.
“We would see each other a little bit at midnight,” she says, laughing.
But working the Thanksgiving holiday was more normal than not for Velez. She usually works that holiday so she can spend Christmas Eve (her birthday) and Christmas Day with her husband and children. What was different this year was that the usual dinner potluck she would have had with her close friends, many of whom also work in medicine, was moved to a virtual celebration. It was also overshadowed by the exhaustion that comes from eight months of battling a pandemic and the anxiety of what she believes is going to be a very difficult winter.
“You live in the hospital world, you see what’s happening with COVID, then you go to the grocery store and you go out places and you see people not doing the right thing,” she says. “It causes so much angst.”
For Velez, it’s been taxing to watch friends post on social media about parties they are having, even as her patients become sick and die from COVID-19. And what is particularly distressing to her is that she sees a disproportionate number of patients from underrepresented and low-income communities.
“They cannot stop working. They have to go to work to make a living and to pay their bills,” she says.
She also worries that many people, particularly younger people, don’t understand how serious the virus can be.
“It’s a disease that is very puzzling to doctors, and it is so new to all of us,” she says. It doesn’t always seem to follow expected patterns. “There are people who are young and healthy who get super, super sick, and there are some who are older with medical conditions who don’t get the severe disease.”
Judging by how many people traveled and gathered over Thanksgiving, Velez dreads the coming weeks.
“I think we’re heading into very, very difficult times,” she says. “It’s horrible when you have to tell someone on an iPad over Zoom that they have to say goodbye because their family member is going to die or has died. That takes a huge emotional toll on everyone.”
Jennifer Keating, MD, JD, psychiatry resident at the University of South Dakota Sanford School of Medicine in Sioux Falls

Keating, who worked her first Thanksgiving as a psychiatry resident this year, would normally have spent the holiday with both her and her husband’s extended families. Instead, she had a smaller dinner with just her husband and 3-year-old daughter.
Since she is expecting a child, she feels fortunate that she can conduct most of her patient care virtually, including the COVID-19 patient she saw on Thanksgiving Day. While she said that her shift on Thanksgiving didn’t feel different from how days have been over the last several months, she does feel a sense of dread about what may come in the wake of people gathering for the holiday.
“I just kind of feel like you’re in this, waiting to see what happens,” Keating says.
As a psychiatrist, she has encouraged her patients to remain hopeful.
“It’s reinforcing that they’re not alone going through this,” she says. “A lot of us are struggling currently.”
Breanna O’Neil, MD, general surgery resident at University of South Dakota Sanford School of Medicine in Sioux Falls

O’Neil arrived at the hospital for her 28-hour shift at 6 a.m. for a busy Thanksgiving Day. She performed several emergency surgeries and had patient consultations — all with a strained nursing staff.
“It’s been hard because the hospital is so full,” she says.
She was grateful to be able to take a short break and share in the Thanksgiving potluck that the nursing staff organized.
Normally, O’Neil would spend Thanksgiving cooking a big meal for her dad and three brothers back in Wisconsin, but she hasn’t seen them since August.
Instead, she took a long nap when she got home before celebrating with her husband and 15-month-old son. Spending time with her son is one of the things that keeps her grounded during the pandemic.
“He’s so young, he doesn’t know anything different,” she says. “Just to see him laugh and play and be happy, it reminds me life can be a lot simpler.”
Robert Goldszer, MD, chief medical officer at Mount Sinai Medical Center in Miami Beach, Florida

Thanksgiving is one of Goldszer’s favorite holidays because it’s one of the few that doesn’t require him to buy presents for anyone, but it’s still a time for eating good food and gathering together with the family.
But this year, instead of cooking a big meal with his two adult children, he and his wife ordered a takeout Thanksgiving meal for just the two of them.
Goldszer spent Thanksgiving morning working as an attending physician with the medical service at the hospital, a shift he doesn’t mind volunteering to take so that other doctors can take the day off.
Though the day carried more stress than it has in the past, especially as his team was concerned for some COVID-19 patients that were admitted that day, he said that overall morale was high.
“There was very good camaraderie [among the staff],” he says. “The patients were very appreciative.”
The hardest part of the day for Goldszer was to witness the negative impacts that social determinants of health had on some of his patients, particularly those who were homeless or didn’t have a support system that allowed them to go home.
“Thanksgiving is a wonderful holiday, but it heightens those things,” he says. “The things you have — your family — some people don’t have that.”
Goldszer and his wife made a point of eating in the dining room, lighting candles, and using special napkins for their Thanksgiving dinner, despite it just being the two of them. It was important to him to mark the day with a celebration to recognize all that he’s grateful for.
Brenda Her, MD, third-year medicine pediatric resident at the University of Minnesota Medical School in Minneapolis

During her Thanksgiving Day shift, Her felt conflicted. She wanted to spend extra time with each of her patients, especially since most of them were not allowed visitors and would be spending the holiday alone, but she was also eager to get home to celebrate with her boyfriend.
Any other year, Her, the oldest of 11 siblings, would spend Thanksgiving with her family and then celebrate the Hmong New Year that weekend at the Xcel Energy Center in St. Paul, where people gather to celebrate the traditions of the Southeast Asian Hmong community.
But both plans were canceled this year because of the risks of the pandemic. Even though her family only lives 15 minutes away, she didn’t want to risk exposing her mother, who is at high risk for serious complications from COVID-19.
Her is all too familiar with the severe impact the disease can have. She says that about a third of the patients she saw on Thanksgiving had COVID-19. She also estimates that of all the COVID-19 patients she’s treated, about a third of them have died.
The news of two promising vaccines that could begin distribution before the end of the year has brought her hope, but she remains anxious about the coming weeks as Minnesota hospitals fill up.
“I think things will be getting worse before they get better,” she says.
Stewart McCarver, MD, emergency medicine physician at Penn State Health Milton S. Hershey Medical Center in Hershey, Pennsylvania

McCarver’s Thanksgiving Day shift in the emergency department wasn’t atypical. In fact, it was a bit slower than a normal day.
“People were busy eating turkey and not coming into the ER,” he says, although he did treat one patient who came in with a piece of turkey stuck in his esophagus.
But McCarver anticipates he’ll be much busier treating COVID-19 patients in the weeks to come. One patient who came into the hospital and tested positive for COVID-19 admitted to the doctors that he had Thanksgiving dinner with his family despite feeling sick.
“I’m sure there are a million cases like that,” he says. “COVID is going to get so bad.”
He had originally hoped to spend Christmas with his son’s family, who was going to travel to Pennsylvania from Texas, but the latest surge changed their plans.
Though he’s bracing for a wave, McCarver hopes that preventive measures could still make a difference.
“We’re prepared to treat them,” he says. “But we’d prefer they not get sick.”
Lauren Jodi Van Scoy, MD, associate professor of medicine, humanities, and public health sciences at Penn State College of Medicine in Hershey, Pennsylvania

A couple of days after working a shift the week of Thanksgiving, Van Scoy came down with a bad cough and she could see that her 7-year-old son was anxious. The inconsistency of schooling in the pandemic has been stressful for him, as he bounced back and forth between school and day care when schools switched to virtual-only classes. Since both of his parents are doctors, attending school from home isn’t an option. He also worries about his parents, even asking Van Scoy to stop seeing patients.
She was relieved when she could tell him that her three COVID-19 tests had come back negative and she was only sick with a “regular” virus.
Van Scoy has faced judgment for putting her two children in day care because of the virus risks, but she’s also been criticized when she’s had to take them into work with her.
“It’s the unexpected. What’s going to happen with my kids if school and day care close? And I still have to work, so I have to figure it out,” she says. “I’m really, really, really grateful to the teachers at the day care centers who have been supportive of health care workers at this time.”
Cassie Shaw, MD, assistant professor of internal medicine at the University of New Mexico’s Health Sciences Center in Albuquerque

For Shaw, the pandemic has hit in waves. Sometimes, she feels used to it. Other times, the gravity of it weighs on her.
As New Mexico has seen a spike in COVID-19 cases and hospitals have gotten busier, it feels real again.
“I’ve got an entire list of patients who are very, very sick, when normally it would be one or two,” she says. “It’s exhausting.”
The week of Thanksgiving, she had several younger patients, including one under the age of 30 with no medical problems but a severe case of the disease. His grandfather died of COVID-19 and his grandmother was in the intensive care unit with it.
“He’s scared,” she says. “He says this is the worst thing he’s ever felt.”
Shaw is scared too. She worries that young, healthy people aren’t taking the virus seriously.
But she’s also been inspired. When one of her patients who had been recovering suddenly took a turn for the worst, she and her entire team rallied around them calmly and professionally.
It made her grateful that she was on a team of hardworking people making a difference.
After her shift, Shaw journaled about her experiences from the day and reflected on why she continues to do what she does.
“It feels like, even though there’s so much of this Thanksgiving that’s not the same, at least I’m spending that time doing something good — taking care of patients.”
