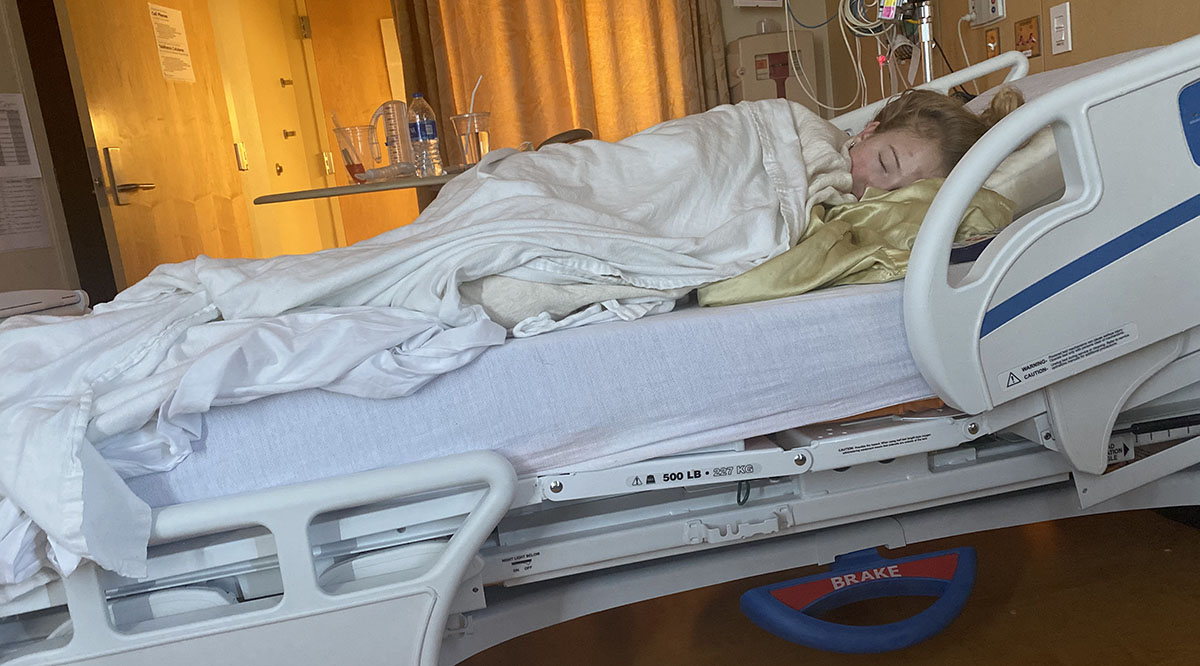
When Haley Bryson’s post-COVID-19 symptoms began, they struck mightily. The 9-year-old from Manassas, Virginia, suffered headaches, earaches, exhaustion, soreness in her chest and throat, and stomach problems so bad they sent her to the emergency department twice. She quickly dropped 20 pounds from her 75-pound frame, according to her mom, Javanese Hailey.
The fourth grader — who previously reveled in performing handstands, cartwheels, and forward rolls — felt sick every day starting in August 2021, just a few weeks after a fairly quick recovery from COVID-19.
“I was really sad because being sick was preventing me from doing a lot of things I like to do” — even arts and craft projects, she says.
Haley, who’s been seen at the Post-COVID Care Program at Children’s National Hospital in Washington, DC, since October, is feeling much better now. But before, she explains, “all I wanted to do was lay down because everything hurt so much.”
Although COVID-19 infections in children are usually not severe, even those with mild cases can suffer from long COVID-19 months later.
And studies suggest that long COVID-19 affects children with the same wide and disturbing range of symptoms as adults, from heart palpitations and “brain fog” to difficulty breathing and painful rashes.
“It’s incredible to me the number of really high-functioning kids who are completely disabled for a period,” says Alicia Johnston, MD, co-director of the Multidisciplinary Post-COVID Program at Boston Children’s Hospital, which has treated over 100 youngsters since launching in March 2021. “The recovery is a long and arduous journey for many kids.”
In recent weeks, COVID-19 infection rates among U.S. children and teens have jumped 32%, and nearly 6.8 million young people have already been infected. As for pediatric long COVID-19 rates, research places them anywhere from 2% to 50%, with some experts suggesting the number is closer to 10%. That means hundreds of thousands of kids and teens will likely be impacted.
But a growing number of pediatric clinics at teaching hospitals — roughly a dozen across the country so far — are working hard to provide relief to young people impacted by this little-understood syndrome.
“It’s incredible to me the number of really high-functioning kids who are completely disabled for a period. The recovery is a long and arduous journey for many kids.”
Alicia Johnston, MD
Co-director of the Multidisciplinary Post-COVID Program at Boston Children’s Hospital
“There’s no one answer, no magic pill that can make all this go away,” explains Alexandra Yonts, MD, who has directed the long COVID-19 clinic at Children’s National since it opened in May. Instead, care often requires a coordinated effort that taps the expertise of various health professionals.
Whatever their specialty, providers feel driven by the goal of getting children healthy. “It’s heartbreaking to see these kids so affected,” Yonts says. “Almost unfailingly, every one of them says they just want to feel normal again.”
What’s going on?
Much about long COVID-19 remains a mystery, and it can be especially perplexing when it appears in healthy young people.
Generally, long COVID-19 — known scientifically as post-acute sequelae of SARS CoV-2 infection — is defined as new, returning, or ongoing problems four or more weeks after an initial infection. No one knows precisely why, but the coronavirus can impair numerous organs, including the heart, lungs, skin, kidneys, and brain.
What’s unclear as well is which young people will be affected and how badly they’ll suffer. Older children seem to fare worse, but that may be partly because of their ability to articulate concerns, says Yonts, who has seen kids as young as 3 in her clinic. Research further suggests that symptoms may recede — and then come back.
They also can last for months on end. That’s what happened to Lilly Downs, a Golden, Colorado, 17-year-old who has been ill for a year and spent two months hospitalized. Her symptoms included a rapid heart rate even while asleep, low blood oxygen levels, and digestive issues that have left her reliant on feeding tubes.
“It definitely has been scary and confusing,” says Lilly, who is being treated in a post-COVID-19 clinic at National Jewish Health in Denver. Perhaps most disturbing were the open skin wounds covering much of her body. “Those hurt so bad I couldn’t sleep.”
“Some doctors even said long COVID doesn’t affect kids. I was out there grasping at straws. [Finding care] has made a world of difference.”
Nicole Nesbit
Parent of 11-year-old with long COVID-19
Long COVID-19 can also spark painful emotional effects, possibly caused by the coronavirus itself or by the strain of physical symptoms. Approximately half the children treated at the Kennedy Krieger Institute’s long COVID-19 clinic in Baltimore suffer from anxiety or depression, according to Laura Malone, MD, a pediatric neurologist there.
“Not being able to participate in extracurricular activities can be isolating, and these activities gave patients a lot of joy before,” adds Malone, an assistant professor of neurology and physical medicine and rehabilitation at Johns Hopkins University School of Medicine. “Some have been very high-achieving students and tell us that they are stressed and embarrassed that school has become so difficult for them.”
Watching their kids contract a baffling syndrome takes its toll on parents as well.
“It was really scary because it felt like no one had any idea how to help,” says Nicole Nesbit, whose 11-year-old son Riddick has suffered intense headaches, fatigue, dizziness, and more since contracting COVID-19 in August.
“Some doctors even said long COVID doesn’t affect kids,” Nesbit adds. “I was out there grasping at straws.” In October, following a web search, Nesbit found care for Riddick at Boston Children’s Hospital. “It has made a world of difference,” she says.
Helping kids heal
Children being treated for long COVID-19 may need care from multiple specialists, including pulmonologists, sleep specialists, pain experts, and rheumatologists.
A clinic’s core team usually determines which types of care are needed after a thorough evaluation, part of which may be conducted remotely.
At Children’s National, for example, the process begins with an intake call that’s followed by a two-hour, in-person visit with specialists from infectious diseases, psychology, and rehabilitative medicine, as well as other departments if needed. Clinic leaders can also provide expedited referrals to other providers, shrinking wait times from weeks to days.
Sometimes, clinics enlist a school resource specialist to help patients navigate any education-related issues, including accommodations. That’s especially valuable since the U.S. Department of Education recognized long COVID-19 as a qualifying disability in July.
Riddick Nesbit knows well how long COVID-19 can interfere with learning. “Sometimes my headaches hurt so bad that I can’t think straight,” says the sixth grader. Since getting treatment at Boston Children’s — including medication adjustments and lifestyle changes like ensuring he stays hydrated — the pain now comes less frequently. Riddick is also doing recommended mental exercises to improve his memory and physical therapy to help with his dizziness.
When it comes to physical therapy for long COVID-19, Johnston recommends using providers who understand post-viral syndromes that sometimes strike after a condition like mononucleosis. “It’s important to design a graduated program to address what can be incredible deconditioning for these kids, or they risk injury,” she notes. Sometimes, that may mean just walking to the mailbox until doing so can be tolerated without exhaustion before moving up to the next level of effort.
Some young post-COVID-19 patients with loss of smell may benefit from “physical therapy for their noses” — olfactory training — that calls for sniffing oils like eucalyptus and lemon twice a day, explains Marc Thorne, MD, MPH, an otolaryngologist at the Pediatric Post-COVID Syndrome Clinic at Michigan Medicine’s C.S. Mott Children’s Hospital. The approach isn’t a guaranteed solution, he says, but it’s worth trying since loss of smell can harm kids' desire to eat and their nutritional intake.
At Michigan’s clinic, breathing issues are a major focus — especially treating children who experience shortness of breath when active, says pulmonologist Carey Lumeng, MD, PhD. “We don’t know whether this is asthma brought out by COVID and it might go away in a year, or if it’s something else that might be lifelong, but many of our patients respond to asthma treatments like inhalers,” he says.
Whatever care entails, patients say they particularly value a sense of being taken seriously.
“Since I’ve come to National Jewish, I have not seen a single doctor that hasn’t been engaged or didn’t believe me,” says Lilly. “I sometimes even call them helicopter doctors because they’re so protective. I feel super-supported.”
Figuring out the best care for kids
Creating care for kids affected by long COVID-19 is no simple matter.
Though post-COVID-19 clinics for adults have popped up in nearly every state, those rarely are meant for children. In fact, existing pediatric long COVID-19 clinics often field appointment requests from families hundreds of miles away.
But staffing clinics sometimes can be tough. “When we opened our clinic in April, we didn’t know if we would get five patients or 5,000,” says Lumeng, who notes that the number is closer to 100. “It was hard to predict manpower needs, and we still have additional work to do besides long COVID.”
At Children’s National, Yonts points to another coverage concern. “Most of our patients so far are from very medically literate, connected families and not necessarily from the demographic groups most affected by COVID. We suspect that Latinx, Black, and other underserved communities have large numbers of children experiencing long COVID, and we’d like to be able to reach out to them.”
“I do feel scared sometimes that I won’t get better, but I always try to stay positive.”
Haley Bryson, age 9
Looking ahead, Yonts also hopes to help bolster care by improving providers’ understanding of long COVID-19. Together with the National Institutes of Health, researchers at Children’s National will track up to 1,000 patients age 21 and younger who tested positive for the coronavirus to monitor their physical and mental health for three years and compare them to uninfected household contacts.
Meanwhile, providers emphasize that the best way to prevent long COVID-19 is to prevent COVID-19, and they strongly urge vaccination. “My goal is to not have a clinic anymore,” says Lumeng.
As for those kids already affected by long COVID-19, they’ll need to keep working toward recovery. Haley, for one, is determined to get better. “I do feel scared sometimes that I won’t get better, but I always try to stay positive,” she says.
