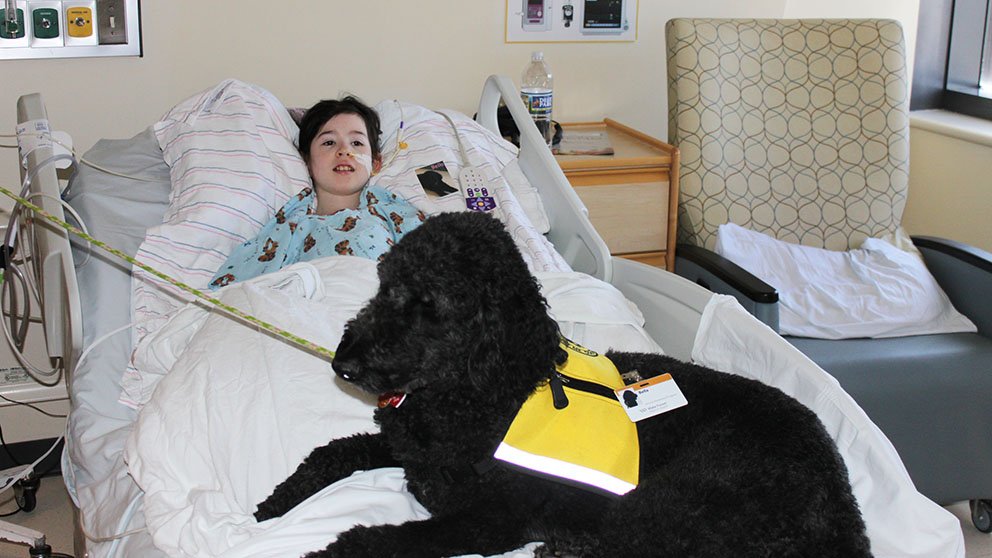
Last year, at age 12, Morgan Lehmkuhl was diagnosed with stage 4 Hodgkin lymphoma. Since then, she’s undergone a stem cell transplant and numerous chemotherapy treatments. Through it all, staff at the University Hospitals Cleveland (UHCleveland) Medical Center have been “great,” she says. But Morgan saves much of her enthusiasm for some of her favorite visitors: dogs from the hospital’s Pet Pals service.
“A dog will come sit on my bed and spend a lot of time with me. I’ll pet it. I’ll give it a treat or ask it to do a trick. One will even play peek-a-boo [by] putting its paws up over its eyes,” she says. “My dog at home brings me lots of comfort, and it’s like that when I see a dog at the hospital,” she explains. “You just forget about all your problems.”
Morgan’s canine helpers join a long history of service. In fact, as far back as 1919, dogs were used with psychiatric patients at St. Elizabeths Hospital in Washington, D.C. But in recent decades, the use of dogs in hospitals has exploded, experts say. Now, the vast majority of children’s hospitals offer canine companionship, and a growing number of adult hospitals provide visits as well.
“The field has been growing exponentially,” says Allison Proctor, MSW, animal visit and therapy program coordinator at Children’s National Health System in Washington, D.C. “It’s gained a lot of traction in the past 15 years because of having more of an evidence-based backing, but we haven’t reached the apex yet.”

What’s more, as canine visits have grown in number, providers also have expanded how dogs help. Increasingly, they’re being used as treatment tools in occupational therapy, physical therapy, and other forms of care. The next frontier may even be welcoming them into post-op units and the intensive care unit (ICU).
Of course, putting dogs in hospitals is no simple matter. Proponents have had to work hard to address staff concerns about hygiene, safety, and other issues. But staff often come to adore the dogs, and canine squads also offer much-needed stress relief to residents and medical school students.
No matter how they’re used, canine companions will always lap up opportunities to spread joy, dogs’ handlers note. “I think she loves it,” says Karen Pranikoff of her dog Bella, who goes to the children’s hospital at Wake Forest Baptist Medical Center. “I think she senses the joy she brings when she visits.”
Joining a proud pack
Before she could become a hospital volunteer, Sadie had to fill out a 7-page application — or her owner did. And that was just a tiny part of the process.

The approval steps usually go something like this: Spend many hours in a training club taking classes such as “canine good citizenship.” Then pass tests and get certified by a recognized organization like Pet Partners or Therapy Dogs International. Then, once certified, jump through each hospital’s own hoops — like staying calm when suddenly faced with a clown or a bunch of balloons.
But all the work is worthwhile, experts say. Indeed, studies on animals in health care facilities point to several benefits, including improved pain management and mobility. For example, one study comparing volunteers visits with volunteer-plus-pup visits found that dogs’ participation better reduced patients’ stress hormones, blood pressure, and feelings of anxiety.
Once dogs are accepted, hospitals connect them with patients in different ways. Depending on the program, dog-handler teams may go door-to-door, patients may request a visit, or a physician may provide a referral for care-related services. In addition, about a dozen dogs have been trained by the Massachusetts-based group NEADS World Class Service Dogs to work as teammates with specific health care professionals.
“Thirty years ago you wouldn’t have heard much about dogs at all. Now … you even see llamas, miniature horses, and rabbits.”
Allison Proctor, MSW
Children’s National Health System
Proctor remarks at the extent to which dogs have been integrated into hospitals. “Thirty years ago you wouldn't have heard much about dogs at all," she says. "Now you see them in so many hospitals. Sometimes,” she adds, "you even see llamas, miniature horses, and rabbits.”
Canine care providers
Even the simplest canine connections can have big benefits, says Suzanne Thompson, animal assisted activity therapy coordinator at Wake Forest Baptist Medical Center. Take asking a dog to fetch a ball. “[This is] an opportunity to have some control that a patient might not otherwise have in a hospital. They get to direct and praise the dog,” she says. “There’s a sense of empowerment.”
But in some hospitals, dog visits go well beyond basic games and snuggles. At Wake Forest, for example, about half the visits address therapy-based goals. “There are times when a dog can help a patient work on specific skills,” says Thompson. “If so, that’s overseen and charted by someone like a licensed recreational specialist.”
A patient with memory issues might focus on recalling a dog’s name, and one receiving occupational therapy might work to grasp a dog’s toy, explains Sheryl Katzanek, who directs the office of patient advocacy at Boston Medical Center (BMC) and runs its dog program. “Patients will often participate in therapy longer when a dog is involved. It’s pleasant. It’s a helpful distraction.”
“I find we get almost as many requests for dogs to be with staff as with patients and family. That has been a benefit of this program that I never would have imagined.”
Sheryl Katzanek
Boston Medical Center
At BMC, dogs also have worked successfully with patients who have substance use disorders and mental health conditions. Katzanek describes one adolescent who suffers from intense anxiety. “The young lady sits on the floor with Rylie, just petting her,” she says. “The therapist reports that Rylie makes the patient calmer and much more communicative.”
Rylie also helps soothe stressed students and staff, Katzanek adds. The BMC program, like others, brings dogs over to the medical school during exams and can send dogs into resident workrooms at particularly stressful times, like following the death of a patient.
Staff tend to love their four-legged visitors, says Katzanek. “We are a large trauma center, and our mission is to serve the underserved. We see a lot of life realities that are not happy,” she notes. “I find we get almost as many requests for dogs to be with staff as with patients and family. That has been a benefit of this program that I never would have imagined.”
Doggedly handling obstacles
No growling. No accidents. One strike and you’re out. Those are among the dog-related hospital rules designed to ensure the safety and comfort of staff, visitors, and patients.
At Wake Forest, dogs have to be taking a flea and tick preventative and must fast for two hours prior to arrival. And if an elevator is occupied, the dog can’t board without the other passengers’ say-so.
In fact, hospitals usually provide volunteers with highly detailed orientations, including rules about being accompanied by a staff member and areas that are off-limits.
“We review things like boundary issues, what to say, what not to say," explains Barbara Nalette, UHCleveland’s director of volunteer services. “Owners may be tempted to ask patients things like, ‘How are you today?’ But they don’t know the patient’s situation. We remind them to keep the conversation focused on the dog.” Also, volunteers must steer clear of rooms where someone is allergic or seems hesitant about a dog visit.
Such efforts have helped win over many naysayers, she notes. “In the early days of the program over 25 years ago, there were lots of concerns. People would say dogs don’t belong in a hospital. But so many fears have proven unfounded.”
“We follow many policies and procedures based on research on animals in hospitals,” she explains. “For example, we’d always have someone who was interacting with a dog use a hand sanitizer afterwards. Now we know that MRSA has been found on dogs’ coats, so we also have people clean their hands before touching the animals as well.”
Today, the dogs are hugely popular, she says. “If we had four times the dogs,” she notes, “we still couldn’t meet the need.”
Sniffing out future options
Looking ahead, experts see increasing opportunities to use dogs — and cats and miniature ponies and other furry friends — in hospitals.
Children’s National, for example, got its first full-time animal coordinator this year. In that role, Proctor says, she began by reaching for low-hanging fruit.
“Most facilities start animal-assisted work with patients who are low risk, but people are exploring the next step, like dogs visiting the ICU. That’s in part because there’s increasing evidence that the benefits associated with dogs — like a faster recovery rate — may outweigh the risks,” she says. For example, Johns Hopkins Medicine already brings dogs to visit or work with one or two appropriate ICU patients each month.
“Also, using animals in more intensive interventions is where animal-assisted therapy is going,” Proctor adds. She notes the use of dogs to help patients with eating disorders at her hospital, and the military’s widespread use of therapy dogs with PTSD patients. “Animals are going to get pulled in a lot more to help with harder cases,” Proctor predicts. “Animal-assisted therapy is great for so many people, but it’s especially helpful for populations where other modalities have failed.”
Whatever direction the field takes, Katzanek sees dogs as integral to helping patients — and staff. In fact, she says, another unexpected benefit is the role dogs play in teambuilding at BMC.
“We’ll walk in with a dog and the whole team — medical students, residents, attendings — will drop to their knees together. Dogs humanize us. They let us step out of our professional, serious selves for a few minutes,” she says. “You see someone like the chief of the service differently after that. Dogs are the great equalizer.”
