Editor’s Note: Throughout 2016, AAMCNews will explore how medical schools and teaching hospitals are educating the next generation of physicians in an environment of discovery and innovation.
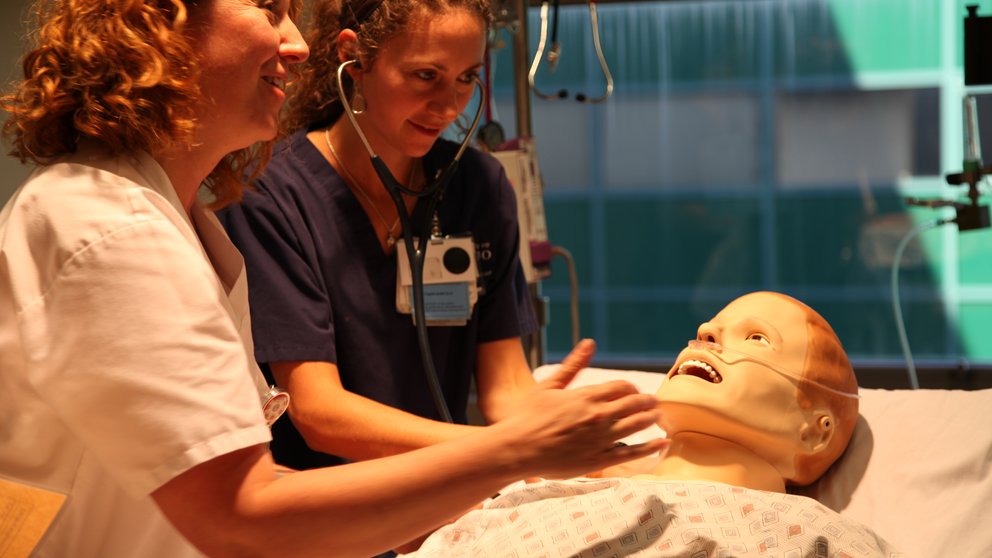
It is known simply and ominously as the “horror room.” Filled with examples of medical errors and potential health care hazards, the room provides an eye-opening lesson in patient safety to all incoming residents at the University of Chicago Medical Center. The room is set up like a hospital inpatient room to help residents look for potential safety errors in a controlled environment.
“When you walk in, you feel hyperaware of having to find the problems,” said Lauren Feld, MD, a first-year internal medicine resident at the medical center. “The experience empowers you the next time you enter a patient’s room. You feel more focused on finding problems, fixing them, and being proactive about it.”
Among the many errors and hazards Feld found were a hand sanitizer dispenser that was empty and a name in the medical records that did not match the name on a mannequin’s wristband. According to Jeanne Farnan, MD, MHPE, assistant dean for curricular development and evaluation at the University of Chicago Pritzker School of Medicine, the point of the horror room, which first launched in 2011, is to heighten residents’ situational awareness. In other words, Farnan said, the hands-on experience opens residents’ eyes to “hazards that we might have begun to overlook as everyday fixtures in a hospital.”
The horror room is just one example of the innovative ways residents are learning about patient safety and quality care. Both the AAMC Core Entrustable Professional Activities for Entering Residents and the Accreditation Council for Graduate Medical Education call for residents to be trained in patient safety.
According to a 2013 article in the Journal of Patient Safety, the annual U.S. toll of medical error-related premature deaths at medical schools and teaching hospitals is more than 400,000.
“When we talk about safety and risk reduction, it’s about creating a culture in which people feel confident that they can raise their hands when something doesn’t feel right.”
David Mayer, MD, MedStar Health
“Health care is a high-risk industry,” said David Mayer, MD, vice president of quality and safety at MedStar Health, a nonprofit health care organization headquartered in Columbia, Md. “When we talk about safety and risk reduction, it’s about creating a culture in which people feel confident that they can raise their hands when something doesn’t feel right. That’s critical to achieving our goal of zero mishaps.”
More than a decade ago when Mayer was serving as an academic dean at the University of Illinois College of Medicine at Chicago, his interest in integrating patient safety into the curriculum led him on a literature search for promising strategies. He found less than a handful of examples. In response to the dearth of information, he and fellow experts founded the Telluride Patient Safety Educational Roundtable in 2005 to catalyze the development of patient safety education. By 2010, the roundtable had morphed into the Telluride Patient Safety Student and Resident Summer Camps, an immersive, weeklong experience in safety that now welcomes hundreds of students and residents each summer.
Anne Gunderson, EdD, MS, is bringing her patient safety expertise to Medstar Georgetown University Hospital, where she serves as a professor and associate dean for innovation in clinical education. Today, the first group of Georgetown interns and fellows is taking part in concentrated patient safety learning with a long-term goal of building out a safety curriculum during residency, she said. The experience begins with three half-days of dedicated learning during residents’ orientation and goes on to use techniques such as storytelling, gaming, video learning, and breakout sessions. Starting in 2016, Gunderson noted, every resident at Georgetown will leave with a certificate in leadership that includes training in patient safety.
“We need to sit down and look at the big picture, from medical students to practicing physicians. There needs to be a national curriculum on patient safety so that every academic medical center, every medical school doesn’t have to start from scratch,” said Gunderson.
Many medical educators are taking an interprofessional approach to patient safety. At Duke University Schools of Medicine and Nursing, medical students transitioning into residency and nursing students about to receive their RN, jointly participate in six hours of patient safety learning. With so many medical errors rooted in miscommunication, the idea is that learning to work as a team will have inherent positive benefits for patient safety, said Alison Clay, MD, an assistant professor of surgery and medicine.
Medical and nursing students often gain unique insights into one another’s thinking, Clay noted. For instance, during the reflective component, nursing students often respond that they feel more responsible for a patient’s care, while medical students are less likely to speak up about a potential mishap, with many fearing it could jeopardize their residency placement.
“If we only teach safety in our individual silos, we don’t acknowledge the roles we play in preventing errors,” Clay said. “It’s hard to know how important [interprofessional] training is until you make it happen the first time.”
At Johns Hopkins Medicine, the Armstrong Institute for Patient Safety and Quality offers about 20 different learning experiences in safety and quality, from a five-minute video on error reporting systems to a nine-month leadership academy, according to Melinda Sawyer, MSN, RN, assistant director of patient safety. The academy accepts about 30 applicants each year, including residents.
“Residents bring a powerful front-line physician voice that informs us what’s happening and what are some of the challenges to achieving quality and safety,” Sawyer said. “They bring so much value to our work.”
Back at the University of Chicago Medical Center, incoming residents have less than 20 minutes to review a door chart, read through a patient’s history, and identify potential hazards inside the horror room. Farnan said the low-cost, easily replicable technique is leading to increased situational awareness and hazard mitigation only one month into internships. “Residents walk away feeling like they can use this experience the very next day,” she said.
This article originally appeared in print in the March 2015 issue of the AAMC Reporter.