Earlier this summer, a 45-year-old man showed up in our emergency department in Los Angeles with severe stomach pain. After waiting several hours in the noisy, packed waiting room, David (not his real name) was assigned a hospital bed in the hallway. Still in severe pain despite his pain medications, he attempted to distract himself by scrolling through his phone, staring at the wall, closing his eyes, and covering his ears while waiting to be seen by the surgical team.
Once the team arrived, they performed a physical exam, reviewed his imaging, and told David that he had appendicitis and needed emergency surgery. But at this point, after being exposed to several hours of background noise, David had reached the point where he could barely understand what the physician was telling him. He could tell that the team genuinely cared about him, but he struggled to hear their words. David has hyperacusis, a rare hearing disorder that makes ordinary sounds seem intolerable; noisy places, like the emergency department, can be almost painful.
How do we know this? David was our patient, and when we noticed that the noise was causing him discomfort, we advocated to move him to a quieter place and offered him earplugs.
While David’s particular condition may not be common, his experience is. Many people with hearing loss or disabilities that heighten sensitivity to sound struggle to hear in the loud, often chaotic environment that is the hospital. Even those without hearing disabilities may suffer amid the incessant beeping of monitors, the frequent alarms, and the competing conversations happening all around them.
How loud is the hospital?
The World Health Organization, International Noise Council, and Environmental Protection Agency have proposed noise limits for hospitals ranging from a 35-45 A-weighted decibel [dB(A)] level during the day to a 20-35 dB(A) level at night. Despite this recommendation, numerous studies have found that noise levels throughout hospitals at all times of day significantly exceeded this limit. For example, one study from Johns Hopkins Hospital found a daily average sound level of 50-60 dB(A) (analogous to a crying baby or vacuum cleaner), as well as a trend of increasing noise levels over the past 45 years. A 2021 systematic review of 33 studies examining environmental noise in hospitals worldwide found indoor noise levels ranging from 37-88.6 dB(A) during the day and 38.7-68.8 dB(A) in the evening. These noise levels were measured in a wide range of settings, including intensive care units (ICUs), waiting rooms, private rooms, dental clinics, infusion centers, and emergency rooms. Operating rooms (ORs) often surpass 60 dB(A), with peak noise in maxillofacial ORs exceeding 115 dB(A) (equivalent to a siren, firework, or rock band).
The impact of noise
Numerous studies have found that noise pollution in the hospital has detrimental physical and mental impacts on medical staff. Increased noise levels have been associated with heightened anxiety, irritation, increased headaches, more frequent sleep arousal, and malaise at the end of the day. For example, one study found that close to 95% of OR medical staff report experiencing physiologic and psychological effects attributed to excess noise, including fatigue, headaches, inattentiveness, agitation, and restlessness.
Excessive noise in the hospital may also negatively impact clinical care. Studies have demonstrated that noise pollution may interfere with communication among medical team members and, consequently, adversely affect patient outcomes. Excess alarm notifications not only may exacerbate noise pollution but also are associated with increased alarm fatigue and medical errors. For example, research has shown that hospital alarms often provide ambiguous, superfluous, or false information; a 2013 Joint Commission report estimated that 85%-99% of all hospital alarm notifications do not require a clinical intervention. Excess noise (e.g., loud music or conversation) may also distract providers from identifying urgent situations, such as identification of auditory changes in the pulse oximeter tone representing a drop in oxygen saturation.
Noise pollution is also detrimental to the health of patients. Increased noise exposure has been shown to be associated with worsened patient anxiety levels and sleep quality in ICUs and ORs. It may also be a potential environmental stressor for patients at risk for falls. And it may impact patients’ heart rate and blood pressure, as well as length of hospital stay, wound healing rates, and gastric activity.
What contributes to noise pollution?
Sources of noise are common throughout the hospital. In the ICU, these may include conversations [75-81 dB(A)], oxygen equipment [70-77 dB(A)], air conditioning [60-67 dB(A)], respirators [49-72 dB(A)], and alarms [up to 84 dB(A)].
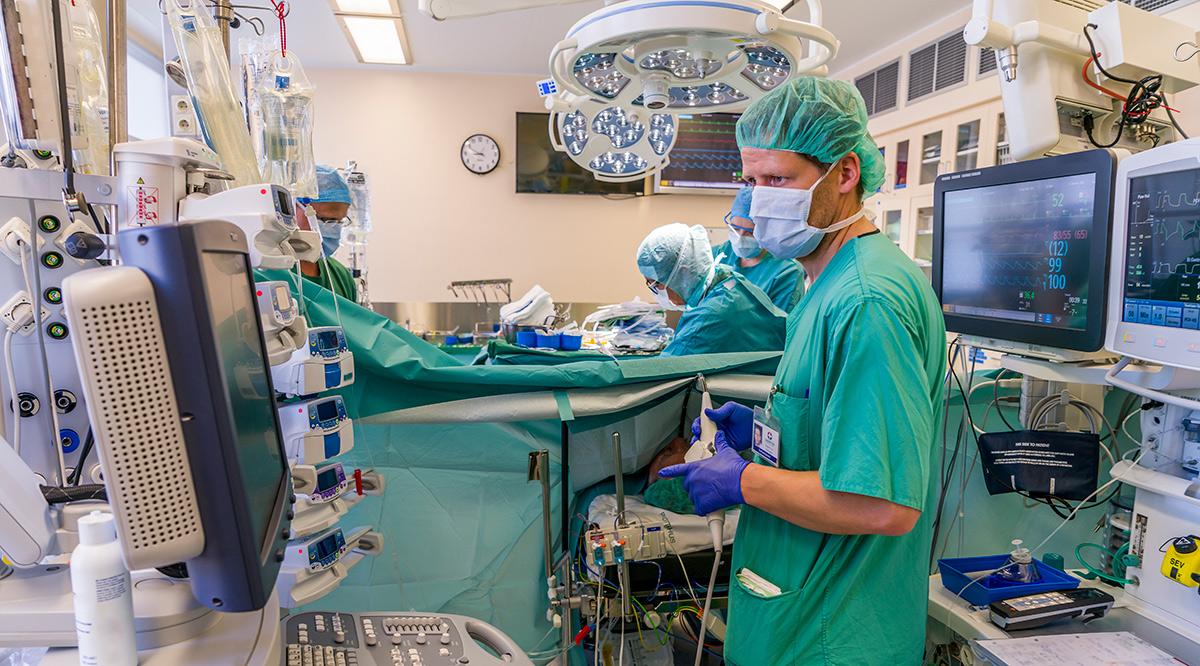
In the OR, sources include suctions [55-60 dB(A)], pulse oximeters [60 dB(A)], and conversations [73-82 dB(A)]. Cautery instruments, pumps, drills, metal instruments, and air-driven tools further aggravate these challenging acoustics.
Loud music is another source of noise. A recent survey of nearly 700 surgeons conducted by Spotify and Figure 1 (an online social networking service for health care professionals) found that 90% of surgeons listen to music while operating. Although some may find music beneficial in the OR, loud music can be distracting, create an unfavorable auditory environment, and mask emergencies.
Within a teaching hospital, the emergency room, ICU, and medical-surgical floors are reported to have the highest levels of noise.
Preventing loud noise exposure improves care
Steps can be taken to prevent constant loud noise exposure. One study found that more than 60% of noise sources in hospital wards are avoidable to some degree. While current research does not show a causal relationship between noise reduction and patient outcomes, we firmly believe that addressing noise pollution will ultimately improve communication and quality of care. We suggest the following changes.
Actively consider the noise level of your environment. Consider employing digital applications to help monitor volume levels. For example, medical staff who have an Apple Watch can use the Noise app to identify exposure to levels that may be harmful to your hearing.
Identify ways to minimize noise. If working in the OR, minimize the use of surgical instruments that may damage hearing. Clamp the suction when not in use or use a suction with an on-off switch. When feasible, have team members wear hearing protection. Observers who are not essential members of the surgical team may opt to step out of the room during particularly noisy parts of a surgery or procedure (i.e., when activating power tools such as saws or high-speed drills). Discourage any unnecessary commotion and lower the volume of music to better facilitate necessary communication among the surgical team members.
Enforce best communication practices. Assume at least one person will not be able to hear verbal communication clearly and adjust accordingly. Maximize use of nonverbal communication and minimize conversations not pertinent to the surgical case, rounds, or patient care. Adopt systems for notifying individuals in the room when to be quiet.
When communicating with patients, silence all background noises, including the television. Ask patients if they have any specific needs and use any assistive technology a patient may have. If applicable, incorporate other learning modalities, including writing important points. Consider implementing a music and quiet rest period protocol for patients; such protocols have been shown to decrease blood pressure, pain, and anxiety levels. Move alarms placed directly by the bedside to a location farther away from patients and use remote monitoring of in-room alarms by nursing staff.
Identify and invest in long-term solutions. Implement low-cost adjustments to noise levels, such as fixing creaky doors and wheelchairs. When feasible, optimize the acoustics of buildings to create a more favorable acoustic environment — for example, reducing reverberation in rooms with high ceilings using noise absorption panels. Collaborate with others to design or implement quieter tools. Consider supplementing existing visual and auditory communication of alarm events with haptic (vibrotactile) displays. The CanaryBox is a medical device that incorporates a smart system to integrate music playing in the OR with vitals from the anesthesia monitor, automatically reducing music volume during critical situations; it has been shown to improve anesthesiologists’ response times to alarms. Establish multidisciplinary educational programs around noise levels. Advocate for institutional or national policies that promote hearing health in hospitals.
As we continue to improve health care and to identify systemic barriers to improved patient care, particularly for communities that are marginalized, we strongly encourage health systems and leaders to address noise pollution. Creating a more favorable auditory environment will facilitate better communication among medical teams, improve the patient care experience, and protect the hearing of everyone in the hospital.