Back in the old days — that is, this past February — Eric Tritch couldn’t imagine why he would need a daily count of all swabs, face masks, gowns, and gloves on hand at UChicago Medicine. Today, as vice president of the supply chain, he and the entire hospital system depend on it.
Every day, Tritch gets an update on more than 1,000 items so that administrators can determine what’s running low, thanks to an intricate inventory system the hospital created as the spring COVID-19 surge depleted supplies faster than anyone had ever seen. In case COVID-19 cases spike again, Tritch says, “We need to make sure we don’t get caught flat-footed.”
Finding new ways to ensure that front-line staff have critical medical supplies is one of many lessons that hospitals have learned about how to improve staff and patient support in a pandemic. While medical discoveries about COVID-19 treatment draw media headlines, the more quiet, systemic innovations focus on creating strategies to keep workers safe and deploying them effectively. That includes coming up with new ways of securing coronavirus tests and personal protective equipment (PPE), managing staff assignments to avoid burning out front-line workers, and giving patients the care they need while preserving hospital resources.
“One of the biggest challenges is the support and well-being of the workforce,” says Tim Dellit, MD, chief medical officer for UW Medicine, which includes the University of Washington (UW) School of Medicine. “They have to feel safe and confident in providing care. And they have to feel safe and confident that they’re not going to go home and infect their families.”
Meeting that challenge requires “a bundle of practices,” he says.
Staff Safety
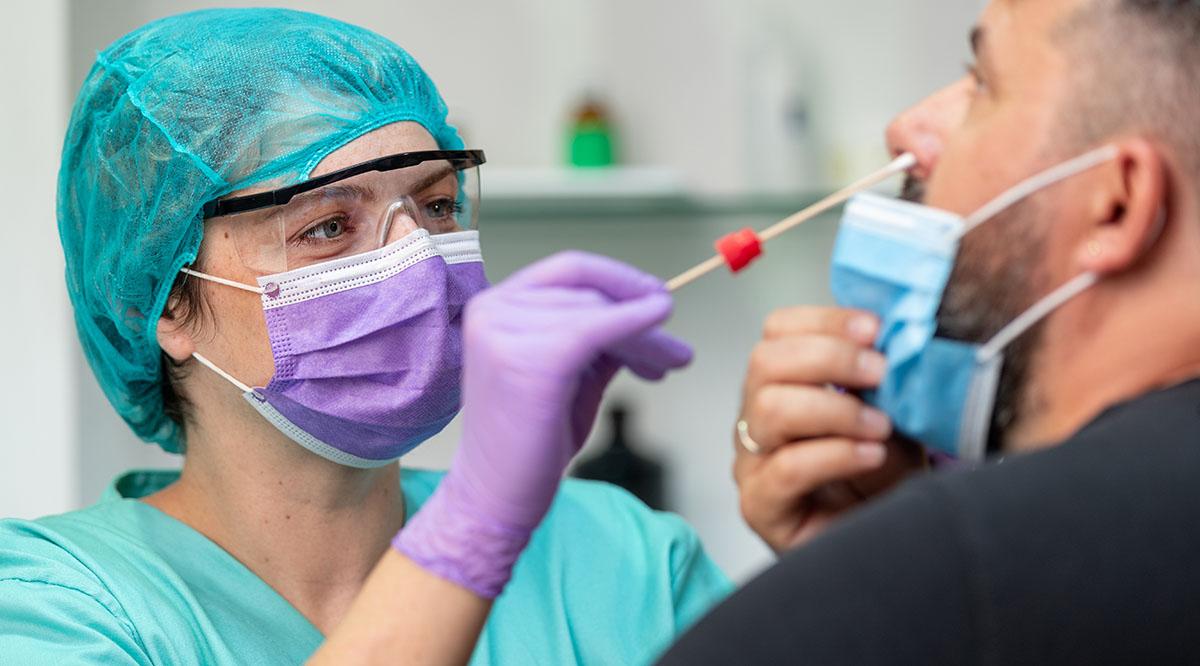
Get creative to secure test supplies: With testing supplies limited in many parts of the country, and with backed-up commercial labs sometimes taking more than a week to return results, some academic medical institutions have found ways to produce and process tests in-house to deliver quick results. UCLA Health in Southern California and UW Medicine in Seattle are using tests developed by their university labs.
“Creating that testing capacity was a game-changer,” says Robert Cherry, MD, chief medical and quality officer at UCLA Health. “That allows for the staff to feel comfortable.”
In Dallas, Texas, the Parkland Health and Hospital System has diversified the testing run by its own lab by purchasing equipment and supplies to collect and analyze test samples on three different platforms, says Chief Clinical Officer Roberto de la Cruz, MD. Every day, the hospital system decides which tests to use based on its supplies for each platform.
“We know we can’t depend on one approach,” de la Cruz says.
Screen almost everyone, a lot: Hospital systems (such as UCLA Health) have made testing part of their routine coronavirus screening of all employees, as well as patients in certain settings, such as anyone who checks in to the emergency department, all inpatients, or all surgical patients (including outpatients).
UCLA Health’s screening process includes posting staff at each entrance to ask everyone entering the hospital about possible symptoms and take their temperature before allowing them in, Cherry says. Hospital staff can start their own screening process before they come to work by tapping into a smartphone app to answer questions about their health conditions. Those who might have coronavirus symptoms are steered to a call center for further assessment and determination of next steps, he says.
Take control of PPE supplies and use: With PPE sometimes in short supply, hospital leaders say it’s essential to continually develop secure supply chains, even during lulls in COVID-19 cases.
At UChicago Medicine, Tritch saw that the standard process of projecting supply needs based on traditional historical usage wasn’t sufficient during the COVID-19 surge. His team created a system that also factors in usage from the previous day and the previous week, then uses those figures to calculate how many days the current supply of each item will last. Each day, he sends an inventory report to key hospital leaders that focuses on 90 of the most critical supplies.
Tritch says UChicago Medicine also found new suppliers, including from overseas, in part by making connections through its board of directors and alumni; set up a freight forwarding program to efficiently get that material to the hospital; and established a new process to solicit and manage supply donations from businesses.
Some hospitals tapped into the special expertise of their universities to create their own PPE. “Leveraging the innovation that’s already in the academic health system is a huge resource,” explains Dellit.
Dellit says a cross-university team at UW used a prototype face shield developed by a private designer to produce 3D-printed face shields for UW Medicine, as well as designs for face masks, gowns, ventilator parts, and specialized boxes to shield clinicians when intubating patients. PPE was produced through similar collaborations around the country, including between Emory Health and the Georgia Institute of Technology, both in Atlanta, and between UVA Health and the University of Virginia School of Engineering and Applied Science in Charlottesville. The latter project, initiated by a query from a nurse at UVA Health, grew into a multisector effort — involving dozens of faculty, local citizens, and businesses — that churned out thousands of PPE products.
With precious PPE in hand, hospitals must also ensure that staff use it correctly. Parkland created a separate entrance and exit to each COVID-19 unit, placing staffers at each point to monitor the donning and doffing of PPE, de la Cruz says.
“It is really helpful for the staff to feel that confidence that they are well-protected and that someone is monitoring them to be sure they are doing it correctly,” de la Cruz says.
Staff Management
Expand staff capacity: When NYU Langone Health in New York City found its staff overwhelmed at the start of the spring wave, administrators put out word throughout its system for any doctors, residents, nurse practitioners, and physician assistants who’d be willing to help with patient care and administration. The huge response led to the creation of what NYU Langone called the COVID Army.
“We couldn’t have done it without them,” says Katherine Hochman, MD, associate professor in the Department of Medicine at NYU Grossman School of Medicine.
“We mobilized so many people in such a short amount of time,” she says. “We were able to take care of an extraordinary number of patients, and we were able to take care of them well.”
Nearby, at Northwell Health’s Long Island Jewish Valley Stream Hospital, the COVID-19 surge doubled the average patient-to-nurse ratio in the intensive care unit (ICU), with each nurse managing four patients instead of two, says Darryl Adler, MD, associate director of the ICU. Although the unit borrowed staff from elsewhere in the hospital, the nurses “were just treading water.”
The hospital brought in traveling nurses as well as physician assistants on contract to relieve the load in the ICU and elsewhere, Adler says.
“If this were to happen again, we’d have a bigger pool of physician assistants and nurse practitioners, both from within the system and outside services,” Adler says.
Cost and supply could pose a challenge: Some agencies have reported doubling or tripling their nurses’ weekly rates during surges of COVID-19.
Spread out staff responsibilities: After the spring outbreak subsided, leaders at UChicago Medicine got feedback that raised concerns about the risk of burning out certain staff who provided much of the front-line COVID-19 care — especially early- and mid-career physicians and those in critical care specialties, says Tipu Puri, MD, associate chief medical officer for clinical operations. The staffing decisions “were understandable,” he says, for reasons that included protecting workers “who might be more vulnerable to the impacts of the disease.” But as they prepare for a possible second surge, Puri says, “We need to figure out how to involve everyone.”
The health system is considering a tiered staffing model — similar to one implemented at Hackensack Meridian Health (HMH) in New Jersey, says Chief Physician Executive Daniel Varga, MD. Under that model, nurses from around the hospital were deployed to an ICU to work under the direction of a critical care nurse, and doctors (such as general surgeons and ambulatory internists) were deployed to work under the supervision of a critical care specialist.
“A general internist is probably not the optimal person to be managing [oxygen] vents and running lines, but they’re really effective at doing physical exams and obtaining data,” Varga notes. That, he says, freed up critical care specialists to focus on their special skills.
Patient Management
Weigh the pros and cons of COVID-19 units: Isolating COVID-19 patients in dedicated units — and assigning certain staff to work only in those units — provides advantages but also presents drawbacks.
Because patients at UW Medicine were pooled into cohorts based on test results, the staff “knew who was COVID-19 positive and knew who was not,” Dellit says. “That made a huge difference in relieving anxiety.”
At UChicago Medicine, the approach preserved PPE because the staffers assigned to work only with a COVID-19 cohort kept one set of equipment on for most of the day, Puri says. In addition, the cohorts can pay dividends after coronavirus cases subside and hospitals resume more routine procedures.
“Being able to create COVID-positive and COVID-negative spaces on the basis of testing has been reassuring for people returning for routine care,” says Varga at HMH.
Yet UChicago Medicine would rethink how quickly and broadly to employ that approach if a surge returns, Puri says.
“While it was very effective, it put a lot of burden on a handful of providers who would go into those COVID units and be there all day,” he says. “If the COVID unit wasn’t full, then you have staff capacity that isn’t being utilized because that provider is staying in the COVID unit. They can’t go take care of a non-COVID patient.”
Find ways to keep patients out of the hospital: The creation of temporary field hospitals — by erecting tents in parking lots and parks, for example — has helped hospitals handle patient overflows and focus more of their resources on the more severe cases. As clinicians continue learning about the disease progression and treatments, they see opportunities to treat more people out of hospitals.
“Once a patient is requiring a lower level of care, can we move them out of the hospital to another setting that’s safe?” Puri wonders. “Can we create facilities where we can transition patients and maintain our higher acuity beds in the hospital” for both COVID-19 and other critically ill patients?
Nevertheless, he notes, “there are only so many beds you can create.”
With that in mind, HMH is exploring the use of more “hospital at home” models for less severe cases if the COVID-19 patient load swells again, Varga says. He says that might require people to have some basic medical equipment at home and a trained caretaker (perhaps a family member) who can use that equipment to monitor clinical signs, such as oxygen intake.
Educating the community about preventing the spread of the virus is another way for hospital systems to reduce the load of incoming patients. HMH and Ochsner Health in Louisiana are each formally consulting with local businesses about how to keep customers and staff safe.
Take pressure off the front-line staff: The emergency room staff in hospitals run by the Icahn School of Medicine at Mount Sinai in New York City were so overwhelmed by COVID-19 cases in the spring that they had no time or emotional bandwidth to find patients’ families to give medical updates or to discuss what level of care to provide if the patient was critically ill.
So the Department of Geriatrics and Palliative Medicine established PATCH-24, a 24-hour call center staffed by palliative care physicians who provided family members with medical updates and discussed with them how far to go with medical treatment.
Emily Chai, MD, oversaw the program and made some of the calls: “Tell me about your mom. If she knew what was happening, what would she tell us?”
Those conversations ensured that the staff adhered to the family’s wishes and avoided unnecessary use of critical care resources. Chai adds that the process freed up clinicians’ emotions as well as their time: “A lot of calls were clinicians saying, ‘I’m so sorry. I’m so burned out I can’t think straight.’ The first three to five minutes were therapeutic sessions for overwhelmed front-line clinicians.”