Editor’s note: The opinions expressed by the author do not necessarily reflect the views of the AAMC or its members.
I wake up for my night shift on labor and delivery (L&D) at University Hospitals Cleveland Medical Center and greet my significant other. I’m terrified I’ll bring coronavirus germs home to him and wish we could afford a larger apartment to stay farther apart. I also greet the now familiar pit in my stomach. It comes from the tension between our crucial role as physicians and the risk our job poses to our loved ones and ourselves. It also comes from my sense that my relative lack of clinical decision-making power and experience constrain my ability to contribute.
Make no mistake: I am not complaining, nor do I regret my career decisions. But the true nature of our profession, the risks it entails in the face of a global pandemic, has slapped me in the face, and I am trying to adapt to the impact of the hit.
Not long into my shift, I get a call about a patient who feels a sudden, powerful urge to push, unable to stand the pressure in her pelvis. I quickly get to her room, pull on a pair of gloves, and move the delivery cart into place. I don’t have time, though, to put on my sterile gown as the baby’s head is starting to crown. Thirty seconds later, we celebrate our first birthday party of the shift. The room is less crowded than usual given new limits on visitors, but the cheers are no less ecstatic.
For a moment, everything feels normal.
Then the patient gives out a small cough, turning her head toward me, and I feel incredibly exposed. Normally I wouldn’t care — bodily fluids don’t faze me anymore — but now I feel reckless. I curse myself for not getting to the room fast enough to properly gown. Although the patient likely choked on a sip of water she took, I know it's also possible that she is incubating and spreading the virus. Few patient interactions are more intimate than those on L&D, and each one now seems to come at great personal risk. I make a mental note to not only wear a gown and gloves at all future deliveries, but also a face mask and shoe covers. But then I realize this might soon be against hospital policy as leaders attempt to conserve our ever-diminishing supplies of personal protective equipment (PPE).
As I leave the room, my thoughts are also with the newborn. I wonder about the possibility of his mother transmitting COVID-19 to him and whether it would be life-threatening. I worry about my patients in their first trimester whose fetuses are still developing. Might there be congenital defects or other ramifications for these babies? We have no way of knowing yet. And I’m acutely aware that many months from now when these women go into labor, I will still be dealing with the repercussions of this pandemic.
Back in the team room, out of curiosity I pull up the emergency department (ED) patient list and already see a queue of 30 patients with “cough” or “fever” as their chief concern. I’m secretly thankful I didn’t pursue emergency medicine, but I also wish I were there with my friends and colleagues to share their burden, which must be even greater than mine.
My thoughts are interrupted when I notice a name appear on the patient board next to Triage Exam E, our makeshift area for possible COVID-19 infections. It’s typically my job to cover the triage area on L&D, which functions much like a smaller ED specifically for pregnant women. As I look up her chart, I can’t help but wonder why I am tasked with seeing her when the attending physician must supervise my decisions. I know that I am here both to contribute and to learn, but I am not sure where my medical education fits into the current crisis. I go through my interview questions faster than normal, as if spending a few minutes less with the patient will significantly reduce my possible exposure.
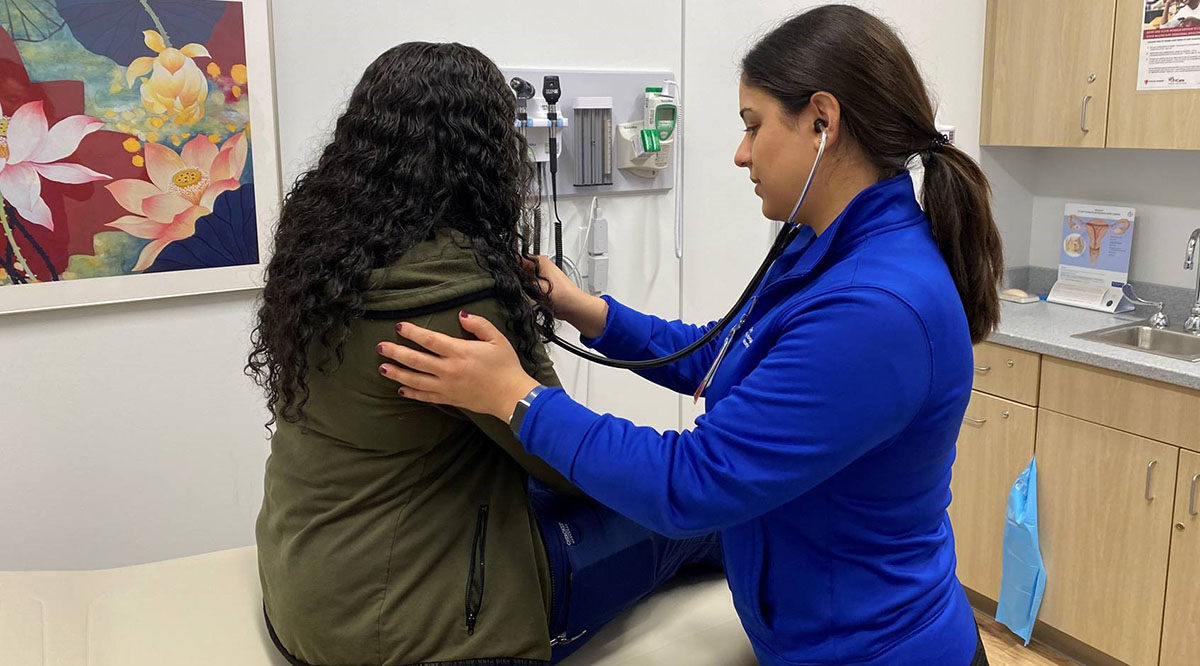
Few patient interactions are more intimate than those on L&D, and each one now seems to come at great personal risk.
When I'm done, I go to the bathroom and wash my hands for 60 seconds and use hand sanitizer in addition. I’m just an hour into my shift, and already I am fearful of being infected for the second time. There's a dull pounding behind my right eye. My brain feels overworked from consciously overthinking every action I, and those around me, take. And I have multiple internal debates about hygiene: How frequently should I sanitize my stethoscope, pager, and computer? Should I shower with the ice-cold water in the call room before leaving in an attempt to wash away the virus and the fear? Am I being proactive, or am I showing signs of hypochondriasis?
At some point in the night, a colleague shows me an article about an otherwise healthy resident who is now intubated in an intensive care unit (ICU) somewhere in California.
Although we get multiple explanatory emails from hospital administration every day about the virus, I still can’t help feeling unprepared.
Throughout the evening, there are several back-and-forth calls with the ED. Making the decision to allow a patient to move from the ED to L&D means potentially putting all other laboring patients at risk. We are trying our best to stick to the hospital-issued algorithms for identifying patients who might have COVID-19. We are supposed to check for respiratory symptoms and rule out other likely, more innocent causes other than the novel coronavirus. But this proves quite challenging. Every pregnant woman experiences some shortness of breath, and anyone with seasonal allergies or mild asthma can have a cough.
There’s also the question of whether the level of obstetric need justifies the potential COVID-19-related risks. Labor can be deceptive, and a woman’s degree of pain from contractions is subjective. Although we get multiple explanatory emails from hospital administration every day about the virus, I still can’t help feeling unprepared.
Toward the end of my shift, I get a phone call about a patient needing direct admission to our service. I’m told she’s been diagnosed with influenza and may also have pneumonia. “Don’t worry when you read the report. It says, ‘Cannot exclude COVID-19,’ but I think they have to say that for liability concerns,” my colleague adds.
Not reassured, I go to meet the patient. Throughout my admission intake, I can’t help but notice that, despite my wearing PPE, there are multiple ways to carry something contaminated out of her room with me. There are no disposable stethoscopes to be found, so I use my own, and I have to bring an ultrasound machine into the room. When I’m done with the intake, I extensively clean every inch of my equipment and take off my PPE, discarding it before leaving the room. Even then, I think about the viral particles that might be swarming in the space between the garbage can and the door. I hold my breath, as if that will help.
Finally, at the end of my shift, I change out of my scrubs. I wash my hands up to my forearms, as if I am scrubbing into surgery, and make my way into the morning air. On my walk home, the sun begins to rise and my mind circles to my family members, who I hope are staying home and infection-free. With celebrations for birthdays and weddings postponed for months, I wonder when I’ll see them next. I have no idea when the country will reach the peak of infection, let alone when the pandemic will die down.
I think about the viral particles that might be swarming in the space between the garbage can and the door. I hold my breath, as if that will help.
I get home and collapse onto the couch. My body has a deep, aching fatigue that begs for sleep, but my mind is still racing. Like the virus itself, the fear of the coronavirus has spread to every aspect of my life. I used to look forward to relaxing after work, but with restaurants and shops closed, my schedule has been stripped down to little more than working and sleeping. Home is no longer an escape; I instead now read COVID-19-related resources that are released daily and watch YouTube tutorials on ventilator settings just in case.
Next week I will switch to the gynecology service, which used to be comprised mainly of elective surgeries that are now canceled. I therefore assume I will be one of the first residents pulled to work in the ED or ICU if needed. I have both a thirst to prove myself and a deep terror at the prospect of this. It's certainly realistic to expect that I’ll be called on if too many other providers are quarantined — if I myself am not quarantined first.
I call my parents in lieu of being able to see them. My mom is frequently trying to find reasons that make me too high-risk to work. I don’t blame her for doing so. I confess that a small part of me wishes I had a reason to stay home and self-isolate like so many others.
But true to my “I always knew I wanted to be a doctor” core, my instinct to serve the public prevails over the instinct to self-protect. As I fall asleep, I remind myself that the only thing scarier than contracting COVID-19 is abandoning my team and my patients in this hour of great need. This does not make me a martyr, nor does it make this period any less daunting. It is simply a job that must be done, a terrifying privilege that I among countless others have volunteered to perform.

