
They devised ways to protect newborns, expanded our understanding of diseases like diabetes, and even mapped portions of the human brain. Along the way, these trailblazing women broke barriers for themselves, underserved patients, and the nation as a whole. In honor of Women’s History Month, we share the stories of 10 female pioneers who changed the face of medicine.
Elizabeth Blackwell, MD (1821-1910): A fabulous first
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
In 1849, Elizabeth Blackwell became the first woman in the United States to be granted an MD degree. Blackwell began her pioneering journey after a deathly ill friend insisted she would have received better care from a female doctor.
Turned away by more than 10 medical schools, Blackwell refused a professor’s suggestion that she disguise herself as a male to gain admission. “It was to my mind a moral crusade,” she wrote at the time. “It must be pursued in the light of day, and with public sanction, in order to accomplish its end.”
Blackwell ultimately attended Geneva Medical College in western New York: Male students there asked their opinion agreed to admit her, thinking the matter a mere prank.
In the years following graduation, Blackwell struggled to find work, but in 1857, she co-founded the New York Infirmary for Indigent Women and Children to serve the poor. The hospital, like the Woman’s Medical College of the New York Infirmary she created in 1867 and many other efforts, was also intended to support and encourage women hoping to pursue careers in medicine.
Rebecca Lee Crumpler, MD (1831-1895): An African American pioneer
The first African American woman in the United States to earn an MD degree, Rebecca Lee Crumpler was inspired by an aunt who took care of many ill neighbors. “I early conceived a liking for, and sought every opportunity to relieve the suffering of others,” wrote Crumpler in her groundbreaking 1883 publication, A Book of Medical Discourses: In Two Parts.
Crumpler gained entrance to the New England Female Medical College in Boston, Massachusetts, after working for eight years as a nurse in nearby Charlestown and receiving letters from doctors commending her. When she completed her education in 1864, she became the only black graduate in the school’s history.
Following the Civil War, Crumpler moved to Richmond, Virginia, to care for formerly enslaved people, where she suffered rampant racism and sexism. Still, the experience taught her a great deal about providing care, Crumpler said, and when she returned home to Boston, she served her patients with “renewed vigor.”
Read more about Crumpler and other African American pioneers here.
Note: No photos of Rebecca Lee Crumpler are known to exist.
Mary Putnam Jacobi, MD (1842-1906): The menstruation myth
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
Mary Putnam Jacobi was interested in biology from the time she was young, and even briefly considered dissecting a dead rat she found to get a glimpse at its heart.
With the reluctant support of her father, renowned publisher George Putnam, Jacobi received her MD degree from the Female (later Woman’s) Medical College of Pennsylvania in 1864. Determined to get a better education than she could in the United States, she also managed to study at l’École de Médecine in Paris — the first woman to ever do so.
Jacobi fought hard for her female peers. She argued for coeducation for medical students, noting that existing women’s medical schools could not provide the same clinical experience as major hospitals. In 1872, she created the Association for the Advancement of the Medical Education of Women to address inequities.
Over the course of her career, Jacobi taught and wrote prolifically about such topics as pediatrics, pathology, and neurology, and she was the first woman accepted into the New York Academy of Medicine. But perhaps her most outstanding contribution was debunking myths about menstruation.
In response to a book by a Harvard professor that argued exertion — including study — during menstruation was dangerous, Jacobi laid out an incisive counterargument proving the stability of women’s strength throughout their cycle. Her paper — brimming with detailed facts, charts, and numbers — won Harvard’s prestigious Boylston Prize and was a powerful tool in women’s fight for better education.
Ann Preston, MD (1813-1872): In the dean’s office
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
As the first woman dean of a U.S. medical school, Ann Preston fought intense hostility to win opportunities for her female students.
Preston first became interested in medicine and physiology while working as a temperance activist in Pennsylvania. After apprenticing with a local doctor in 1847, she applied to all four medical schools in Philadelphia — and was accepted by none.
In 1850, Preston entered the first class of the Female (later Woman’s) Medical College of Pennsylvania, and she went on to become a professor there. When the Philadelphia Medical Society barred female physicians from training in clinics, Preston recruited an all-women board to establish a hospital where women could train. In 1866, she was appointed dean of the medical college.
Eventually, Preston won the right for her students to train at the well-established Pennsylvania Hospital. When the group entered the surgical theater, male students hissed and spat at them — but Preston remained undeterred. In 1869, in response to a campaign to prevent women from studying alongside men, she wrote, “Wherever it is proper to introduce women as patients, there also is it but just … for women to appear as physicians and students.”
Susan LaFlesche Picotte, MD (1865-1915): Devoted to healing Native Americans
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
When she was young, Susan LaFlesche Picotte saw a Native American woman die because a white doctor refused to care for her. Years later, Picotte would become the first Native American woman in the United States to earn a medical degree.
The daughter of an Omaha chief who believed in partnering with white reform groups, Picotte studied in New Jersey and then taught at a Quaker school on the Omaha reservation. There, she helped care for ailing ethnologist Alice Fletcher, who urged her to pursue medicine. In 1889, Picotte graduated from the Woman’s Medical College of Pennsylvania at the top of her class.
When Picotte returned home, she served a population of more than 1,300, often walking miles and working long into the night. She also pursued political reforms, leading a delegation to Washington in 1906 to lobby for prohibiting alcohol on the reservation. In 1913, she achieved a lifelong dream: opening a hospital in the remote reservation town of Waterhill, Nebraska.
Gerty Theresa Cori, PhD (1896-1957): Winning a Nobel
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
Gerty Theresa Cori — the first U.S. woman to win a Nobel Prize in science — and her husband Carl worked as equals, yet they were rarely treated that way.
Gerty and Carl met in Prague during medical school, which she attended at the urging of her pediatrician uncle. The couple moved to Buffalo, New York, in 1922 and began conducting biomedical research at a state institute, where Gerty was warned she’d ruin her husband’s career if the two collaborated. That did not dissuade them, and they went on to publish dozens of papers together.
The pair delved into the body’s use of energy from food, arriving at the Nobel-winning Cori cycle that explained how glucose is metabolized — a key insight for the treatment of diabetes.
Carl was courted by various institutions and became a department chair at the Washington University School of Medicine in St. Louis, but Gerty remained a research assistant. Eventually, in 1947, the same year the pair became Nobel laureates, Gerty was promoted to professor of biochemistry.
Unfortunately, Gerty also developed the rare blood disease myelofibrosis that same year. She fought it for another decade, sometimes in extreme pain, and she refused to give up her research until the last few months of her life.
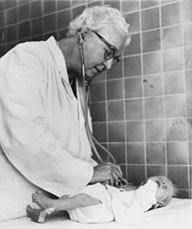
Virginia Apgar, MD (1909-1974): Scoring for babies
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
New parents anxiously await their child’s Apgar score, which is the gold standard for determining the health of a newborn. Virginia Apgar devised that score in 1953, creating the first tool to scientifically assess a neonate’s health risks and need for potentially life-saving observation.
When she graduated from the College of Physicians and Surgeons at Columbia University in 1933, Apgar hoped to pursue surgery. A mentor discouraged her, though, so she studied anesthesiology instead, becoming the first director of Columbia-Presbyterian Hospital’s new division of anesthesia in 1938.
Apgar went on to study the effects of anesthesia, labor, and delivery on a newborn’s health, and she is said to have created her tremendously influential checklist in response to a question from a student. Before the Apgar score, providers had little guidance on assessing and treating infants in their first hours, often losing babies who could have been saved.
In her 50s, Apgar launched a second career, pursuing a master’s degree in public health from Johns Hopkins University and working at the March of Dimes as vice president for medical affairs. There, she drove public attention to such vital issues as how to prevent birth defects.
Former U.S. Surgeon General Julius Richmond once said that Apgar had “done more to improve the health of mothers, babies, and unborn infants than anyone else in the 20th century.”
Patricia Goldman-Rakic, PhD (1937-2003): Brain breakthroughs
 Wikimedia Commons
Wikimedia Commons
Alzheimer’s disease, cerebral palsy, Parkinson’s disease, schizophrenia — scientists’ understanding of these conditions and many more are founded on the groundbreaking research of Patricia Goldman-Rakic.
Goldman-Rakic, who received her PhD from UCLA in 1963, achieved unprecedented insight into the brain’s frontal lobes. Working at a time when the prefrontal cortex was deemed too complex to research in detail, Goldman-Rakic mapped the region and shed light on such crucial functions as cognition, planning, and working memory.
Goldman-Rakic achieved her success by taking a multidisciplinary approach, combining such fields as anatomy, biochemistry, and pharmacology. In fact, when she joined the faculty at the Yale School of Medicine in 1979 — after conducting research at such prestigious institutions as MIT and the National Institutes of Health — she held appointments in several departments, including neurology and psychiatry.
Over her career, she published more than 200 papers and received numerous honors, including admission to the National Academy of Sciences in 1990. She still had much more to contribute, peers noted, when she was struck by a car in 2003 and died two days later.
At the time, Susan Hockfield, provost of Yale University, said of Goldman-Rakic, “Not only was she a dedicated and brilliant researcher, she was also a great and beloved mentor to many junior researchers. Her discoveries and insights into brain function have forever changed our understanding of the mind and brain.”
Antonia Novello, MD (1944-): Fighting for the vulnerable
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
When Antonia Novello became U.S. surgeon general in 1990, her name was etched in two history books: one for Hispanics and one for women.
As a child in Puerto Rico, Novello suffered from a congenital digestive condition that her family could barely afford to treat. That experience motivated her to study medicine and ensure that care was available to all.
After earning her medical degree from the University of Puerto Rico, Novello pursued pediatrics for a while but found the field too heart-wrenching. “When the pediatrician cries as much as the parents do, then you know it’s time to get out,” she said. Instead, she pursued a career in public health, working her way up at the National Institutes of Health for decades and eventually catching the attention of the White House.
As surgeon general, Novello chose to focus on protecting the young and the vulnerable, addressing such issues as underage drinking and cigarette ads that targeted children. Although widely lauded for her achievements, Novello faced a dark moment in 2009 when she pled guilty to using government staff to conduct personal errands back when she served as the New York state health commissioner. Novello claimed she was the victim of former coworkers who accused her unfairly.
Over the course of her career, Novello was committed to battling health inequities among the poor and minority groups. Speaking in 2017 at a health equity symposium at Penn Health, Novello quoted historian Yehuda Bauer, who said, “Thou shalt not be a victim, thou shalt not be a perpetrator, but, above all, thou shalt not be a bystander.”
Joycelyn Elders, MD (1933-): First African American surgeon general
 National Library of Medicine, National Institutes of Health
National Library of Medicine, National Institutes of Health
Joycelyn Elders grew up in a large family in a poor part of Arkansas, and she often missed school to help her sharecropper parents work in the fields. Decades later, she became the first African American surgeon general of the United States and the second woman to hold that position.
Elders did not see a doctor until she was 16 years old, and when she did, she knew she wanted to be one.
After serving in the Army, she enrolled at the University of Arkansas Medical School with funding from the GI Bill, and she graduated in 1960 as the only woman in her class. She went on to become the first board-certified pediatric endocrinologist in Arkansas and to focus on preventing pregnancy among teens with diabetes.
In 1987, Elders was chosen to run the Arkansas Department of Health. In that role, she logged many impressive achievements, including nearly doubling childhood immunizations, expanding the state’s prenatal care program, and increasing supports for elderly and terminally ill patients.
These and many other successes led to Elders’ appointment as surgeon general in 1993. However, Elders was forced to resign in 1994 after coming under fire for several controversial statements on such topics as sex education, masturbation, and the distribution of condoms in public schools.
After leaving her position, Elders returned to her alma mater as a faculty researcher and professor at Arkansas Children’s Hospital. Over the years, she has also crisscrossed the country speaking out about women’s health and other issues. Throughout, she has advocated for those with limited access to care. As she famously said, “Health is more than absence of disease; it is about economics, education, environment, empowerment, and community.”
