It all began innocently enough. A sweet six-year-old took a shine to a medical student who was volunteering in the child’s Ethiopian village. The student was invited to visit the child’s home, and the two soon grew close. Seeing this, the family encouraged the student to consider adoption so the child could escape from a life of poverty. The man declined but certainly wanted to help, and when he got back to the United States, he launched an online campaign to raise funds for the youngster.
But the project hit roadblocks, explains Ruth Berggren, MD, director of the Center for Medical Humanities and Ethics at the University of Texas Health Science Center at San Antonio (UT Health San Antonio), where the student was studying. Other village members couldn’t understand why one child had been singled out for aid. The local organization that handled the financial transfers to the family felt overburdened. And, Berggren notes, the donations undermined the organization’s message that the community could be empowered to care for its own.
“Sometimes, an intended kindness can have unintended consequences,” explains Berggren, who oversees UT Health San Antonio’s global health elective program. “Trainees need to understand that they don’t act in a vacuum when they go to a lower-income country. So many ethical issues can arise.”
Learners' interest in global health experiences has been rising for years. In 2016, 140 out of 145 responding medical schools offered third-year international electives, up from 128 in 2011, according to AAMC data. More than 1 in 4 medical students report participating in such a program, and the numbers are even higher at some schools. In the past decade, 45% of students at the Perelman School of Medicine at the University of Pennsylvania participated in a global experience, for example.
“College students have shown an increased interest in global issues, and they come to medical school expecting to continue that,” says Jenny Samaan, PhD, senior director of the AAMC’s Visiting Student Learning Opportunities™ (VSLO) program, which connects medical and public health students with short-term elective rotations. “So, there’s been a proliferation of programs run by medical schools and nonprofit organizations.”
Certainly, educators recognize the many benefits of short-term experiences in global health (STEGHs) — also called international rotations, global health field experiences, and other titles — for patients and trainees. Participants in such programs are more likely to switch from subspecialty training to primary care, for one, and they report improved diagnostic skills.
Yet efforts in less-resourced places like Botswana, Peru, and Ethiopia can also raise thorny ethical issues. Participants may find themselves asked to perform above their training level, for example. Or they may not be fully attuned to cultural norms or severe resource constraints in the country they’re visiting.
Leaders in academic medicine are paying attention to such concerns. Last year, the AMA Journal of Ethics dedicated a volume to the topic, and in 2018, the American College of Physicians (ACP) published a position paper outlining ethical obligations for STEGHs.
“Trainees need to understand that they don’t act in a vacuum when they go to a lower-income country. So many ethical issues can arise.”
Ruth Berggren, MD, UT Health San Antonio
Meanwhile, medical schools and teaching hospitals increasingly are working to prepare learners to better handle ethical dilemmas and provide care for some of the world’s most vulnerable patients. A key starting point is building strong partnerships that honor a community's own priorities, experts say. Also essential are pretrip trainings, building personal and cultural humility, and recognizing that efforts must fit into a broader landscape of local health care.
“Ethical engagement is not just about feeling good for contributing,” cautions Jessica Evert, MD, a leader in the field and executive director of Child Health and Family International, a nonprofit that partners with the AAMC’s VSLO program. “It’s about determining if an effort honors differences in power and privilege, and it’s about achieving real, sustainable improvements in health and wellness for the community.”
The power of partnerships
Programs that want to provide effective, ethical experiences should avoid veering toward "volun-tourism," experts say. Instead, they should build solid, respectful partnerships with local communities. Some call this “fair trade education,” borrowing from the “fair trade” concept that promotes equity between producers, who are often from lower-income places, and consumers in higher-income nations.
To make sure it was achieving this and other goals, Wayne State University School of Medicine paused its student-run global health trips a few months ago.
Until then, the school’s World Health Student Organization would raise funds, buy medicines, and travel to sites in less-resourced countries. “The students would create pop-up clinics” and organize trips with the help of U.S. nongovernmental organizations, explains Ijeoma Opara, MD, who codirects Wayne State’s new interdisciplinary Global Health Alliance (GHA). “It was students’ responsibility to arrange faculty to accompany them on travel as well as faculty in the host country to provide oversight.”
Now, though, the school is working on extensive changes. “We want to focus on structured, competency-based learning experiences as well as on developing strong, long-term, bidirectional relationships with faculty leadership in host countries,” says Opara.
“Hosts should be fully engaged in program design and defining intended outcomes. Only they really know their resources, their needs, and their capacity."
Jenny Samaan, PhD, senior director, AAMC Visiting Student Learning Opportunities program
Working with partners provides many benefits, including that programs can better respond to local needs and ensure that volunteers don't unintentionally overburden hosts.
“More and more, our program has been involving local partners in selecting and matching students with projects that hosts need,” says Susan Graham, MD, who runs the global health immersion program for University of Washington (UW) medical students. “In the past, we might just wait until students went to the site, and hosts would try to bend over backwards to give them what they wanted,” says Graham.
UW second-year student Shanelle Briggs says local connections were essential for her project in Peru last summer. Her goal was to use WhatsApp to help an attending check on dermatology patients in remote areas. She first took several steps with the help of a local mentor, including interviewing 50 patients to see if they would use the program. “Before we could roll up our sleeves, we did a lot of work to avoid duplicating local efforts and make sure we weren’t imposing our own vision for the project,” she notes.
"Host sites should be co-creators with the sending institutions," adds Samaan. "Hosts should be fully engaged in program design and defining intended outcomes. Only they really know their resources, their needs, and their capacity."
Know before you go
"Predeparture preparation is itself an ethical obligation," declares the ACP position paper on STEGHs.
Such pretrip trainings are at the heart of Penn’s global health program. For starters, students practice for hours in the school’s simulation lab before heading overseas.
“A lot of equipment is different in a place like Botswana, so we want them to get used to that,” explains Andrielle Yost, MPA, the school’s assistant director of global health training. “They also need to practice procedures like blood draws that medical students don't focus on as much in the U.S.”
Penn made these — and several other changes — in response to concerns expressed by hosts and students, explains Yost. Two years ago, clinical trainees started receiving a three-hour pretrip training, and last year, all participants began taking an online ethics training modeled after one created by Johns Hopkins University and Stanford University.

Throughout the training, participants contemplate real-world ethical dilemmas and possible solutions. One scenario unfolds like this: A local clinic doesn't have the recommended medication for a suspected case of meningitis. The trainee could provide an alternate antibiotic, but that risks wasting some of the clinic's reserve of that medicine. What should he do? The answer: Consult with local colleagues who better understand issues like how badly the community might need the antibiotic for someone else.
At Wayne State, predeparture trainings include lessons in the history, language, and culture of destinations, combined with modules from the University of Minnesota’s Global Ambassadors for Patient Safety (GAPS) program. Students’ failure to understand local values can inadvertently cause problems for both patients and providers, notes Kristiana Kaufmann, MD, who codirects the school’s GHA program with Opara.
One GAPS story powerfully conveys that concern. It describes a student volunteering in a Laotian clinic who is approached by a mother and a sick little boy. Unable to speak the language, the student struggles repeatedly to communicate and eventually reaches out to touch the child’s head.
But the boy jumps back with a startled look in his eyes. "I was really confused and starting to panic," the student shares. Later, she adds, she learned that only certain elders have the right to touch a person's head. "At that time in my trip I did not understand that the Hmong believe that the soul resides in the head," she explains.
A humble stance
When working in a less-resourced country, one can unconsciously succumb to a "savior complex," cautions Opara. The goal instead should be to practice both personal and cultural humility.
For one, students should never perform beyond the level of their training — even when asked to do so by patients or providers.
Briggs recalls struggling in Peru when patients approached her for medical advice. She didn't want to ignore them but didn't know how to reply. She wrote about the concern in a required daily online journal and soon got a helpful reply. “Dr. Graham suggested I tell them that I’m not qualified to offer advice since I’ve only finished one year of medical school, but that their dermatologist is highly qualified.”
Madeline Chandra, a fourth-year Penn student who worked in Botswana last summer, appreciates learning to shed some preconceived notions of what constitutes quality care. She was helping treat a very ill patient in a small hospital with slim resources when the man’s heart stopped. “I assumed we’d mobilize everyone to resuscitate, but that didn’t happen,” she explains.
“Later I understood that there was no post-resuscitative care available locally, and it would have taken hours to get him to the city hospital. I realized that doing CPR would have helped my own conscience more than the patient,” she says. "I had to accept that my ideas weren’t necessarily the right ones. Instead, it was about providing the best care with what we had.”
An eye to the big picture
It's essential to look at the broader contexts and implications of a STEGH effort, says Kaufmann. Until recently at her school, she says, "There'd been a history of ‘parachute medicine,’ going to a new, unestablished site without long-standing or deeper understanding of the context. So, we might have been missing important pieces of information about care or even undercutting local efforts."
University of Texas student Jordan Garcia learned about the need to look at big-picture issues from an infestation of tiny fleas.
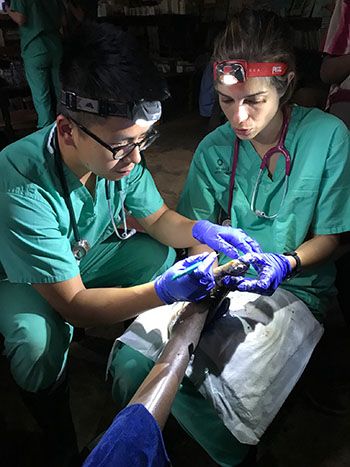
Last summer, Garcia and fellow participants were treating Ethiopian children for Tunga penetrans, which burrow into bare feet and cause terrible itching. The team would carefully clean patients' feet and remove the bugs with a sterilized needle. But they began to worry that the treatment alone was not enough. For one, the children needed adequate shoes in order to heal.
The students discussed their concerns until late one night, Garcia explains, "we put on our boots and showed up in our pajamas at our attending’s door." Ultimately, the students, their attendings, and local partners devised a multipronged solution: raise funds to provide all students with shoes, require that they be worn to school, and treat the environment to prevent a reinfestation of the fleas. “I had started to feel so futile, and I left with so much hope,” says Garcia. “I was so grateful to have faculty with us to discuss day or night the ethics of our intervention.”
The University of Texas has done more to focus on the long view as well: They’ve installed electronic health records in the Ethiopian clinic to track whether their work is actually improving local patients’ health.
Berggren is excited about the future of global health programs. “In fact, I think there’s no better way to get people to care about global health than to immerse them in the reality of these other countries,” she says. Of course, ethics must remain front and center, she adds. In fact, her school has intentionally embedded its global health experiences in its center for ethics.
Samaan agrees, noting that lessons should never come at the expense of those they are meant to help. “We can’t hope to achieve ethical, sustainable experiences unless we start with a solid foundation of mutual respect,” she says.

